Your Free Guide to Medicaid
Your Free Guide to Medicaid
We are privately owned and not affiliated with the government in any way or form.

What Is Medicaid?
Medicaid is a financial assistance program designed to provide affordable coverage to low-income children, pregnant women, families, the elderly and the disabled in the United States, including U.S. territories and tribes.
President Lyndon B. Johnson established the Medicaid program in 1965 as part of an effort to increase access to health insurance in the United States. Today, Medicaid is the primary source of health care for low-income Americans. It is run jointly by the federal, state and local governments.
The federal government requires some benefits and eligibility requirements be included in all state Medicaid programs. However, specific requirements and benefits can vary from state to state.
Refer to the sections called “Medicaid Benefits” and “Medicaid Eligibility by State and Territory” for more information.
Differences Between Medicaid and Medicare
Medicaid and Medicare are both health care programs. However, they have different purposes.
While Medicaid is primarily designed to provide affordable health care for low-income Americans and is operated jointly by the state and federal governments, Medicare is a health care program designed primarily for elderly Americans who are 65 years of age or older.
Medicare is a federal program, which means eligibility requirements and benefits stay the same regardless of location. Medicare requirements are based on work history, spousal eligibility, age, and certain health conditions — not income.
Because Medicaid eligibility includes low-income elderly individuals, some individuals receive both Medicare and Medicaid benefits. Refer to the section called “Dual Eligibility in Medicare and Medicaid” to learn more.
Medicaid Contact Information by State and Territory
| State | Medicaid Program | Department Running Program | Main Phone Number | Office Locator |
|---|---|---|---|---|
| Alabama | Alabama Medicaid | Department of Public Health | 1 (334) 242-5000 | https://medicaid.alabama.gov/content/10.0_Contact/10.1_Medicaid_Contacts/10.1.1_Medicaid_Locations.aspx |
| Alaska | Alaska Medicaid | Department of Health and Social Services | 1 (800) 478-7778 | https://dhss.alaska.gov/dpa/Pages/contacts.aspx |
| American Samoa | American Samoa Medicaid | State Medicaid Agency | 1 (684) 699-4777 | https://medicaid.as.gov/ |
| Arizona | Arizona Health Care Cost Containment System | Department of Economic Security | 1 (855) 432-7587 | https://www.healthearizonaplus.gov/App/Enrollment_Entity_Search_results.aspx?link=Assistor |
| Arkansas | Arkansas Medicaid | Department of Human Services | 1 (800) 285-1131 | https://humanservices.arkansas.gov/contact-us/county-office-map/ |
| California | Medi-Cal | Department of Health Care Services Division | 1 (800) 541-5555 | https://www.dhcs.ca.gov/services/medi-cal/Pages/CountyOffices.aspx |
| Colorado | Health First Colorado | Department of Human Services | 1 (800) 221-3943 | https://www.colorado.gov/cdhs/contact-your-county |
| Commonwealth of the Northern Mariana Islands | CNMI Medicaid | State Medicaid Agency | (670) 664-4890 | https://www.cnmimedicaid.org/ |
| Connecticut | Husky Health | Department of Social Services | 1 (800) 859-9889 | https://portal.ct.gov/dss/About-the-Department-of-Social-Services/Contact |
| Delaware | Delaware Medicaid | Division of Medicaid and Medical Assistance | 1 (866) 843-7212 | https://dhss.delaware.gov/dhss/dmma/locations.html |
| District of Columbia | DC Medicaid | Department of Health Care Finance | (202) 727-5355 | https://dhcf.dc.gov/service/medicaid |
| Florida | Florida Medicaid | Statewide Medicaid Managed Care | 1 (877) 711-3662 | https://www.flmedicaidmanagedcare.com/ |
| Georgia | Georgia Medicaid | Division of Family and Children Services | (404) 657-5468 | https://dfcs.georgia.gov/locations |
| Guam | Guam Medicaid | Public Health Social Services | (671) 735-7519 | https://www.cms.gov/contacts/guam-department-health-care-financing/general-beneficiary-contact/1551566 |
| Hawaii | Med-Quest | Department of Human Services | Oahu: (808) 524- 3370 Elsewhere: 1 (800) 316-8005 | https://medquest.hawaii.gov/en/contact-us.html |
| Idaho | Idaho Medicaid | Department of Health and Welfare | 1 (877) 456-1233 | https://healthandwelfare.idaho.gov/offices |
| Illinois | Illinois Medicaid | Department of Healthcare and Family Services | 1 (833) 234-6343 | https://www.dhs.state.il.us/page.aspx?module=12&officetype=&county= |
| Indiana | Indiana Medicaid | Office of Medicaid and Policy Planning | 1 (800) 457-4584 | https://secure.in.gov/apps/fssa/providersearch/map |
| Iowa | Iowa Medicaid | Department of Human Services | 1 (800) 972-2017 | https://hhs.iowa.gov/about/hhs-office-locations |
| Kansas | KanCare | Department for Children and Families | 1 (855) 643-8180 | https://www.dcf.ks.gov/services/Pages/DCFOfficeLocatorMap.aspx |
| Kentucky | Kentucky Medicaid | Department for Medicaid Services | 1 (800) 635-2570 | https://prd.webapps.chfs.ky.gov/Office_Phone/ |
| Louisiana | Healthy Louisiana | Department of Health | 1 (855) 229-6848 | https://ldh.la.gov/index.cfm/directory/category/158 |
| Maine | MaineCare | Department of Health and Human Services | 1 (800) 977-6740 | https://www.maine.gov/dhhs/about/contact/offices |
| Maryland | Maryland Medicaid | Department of Health and Mental Hygiene | 1 (877) 463-3464 | https://health.maryland.gov/pages/contactus.aspx |
| Massachusetts | MassHealth | Department of Health and Human Services | (800) 841-2900 | https://www.mass.gov/service-details/masshealth-enrollment-centers-mecs |
| Michigan | Michigan Medicaid | Department of Health and Human Services | 1 (800) 642-3195 | https://www.michigan.gov/mdhhs/0,5885,7-339-73970_5461—,00.html |
| Minnesota | MinnesotaCare | Department of Human Services | (651) 431-2670 | https://mn.gov/dhs/people-we-serve/adults/health-care/health-care-programs/contact-us/county-tribal-offices.jsp |
| Mississippi | Mississippi Medicaid | Division of Medicaid | (800) 421-2408 | https://medicaid.ms.gov/about/office-locations/ |
| Missouri | MO HealthNet | Department of Social Services | 1 (800) 392-1261 | https://dss.mo.gov/offices.htm |
| Montana | Montana Medicaid | Department of Public Health and Human Services | 1 (800) 362-8312 | https://dphhs.mt.gov/hcsd/officeofpublicassistance |
| Nebraska | Nebraska Medicaid | Department of Health and Human Services | 1 (855) 632-7633 | https://dhhs.ne.gov/Pages/Public-Assistance-Offices.aspx |
| Nevada | Nevada Medicaid | Department of Health and Human Services | 1 (877) 638-3472 | Northern Office Locations: https://dwss.nv.gov/Contact/Welfare_District_Offices-North Southern Office Locations: https://dwss.nv.gov/Contact/Welfare_District_Offices-South/ |
| New Hampshire | New Hampshire Medicaid | Department of Health and Human Services | 1 (844) 275-3447 | https://www.dhhs.nh.gov/about-dhhs/locations-facilities |
| New Jersey | New Jersey Medicaid | New Jersey Medicaid | 1 (800) 701-0710 | https://www.nj.gov/humanservices/njsnap/home/cbss.shtml |
| New Mexico | Centennial Care | Human Services Department | 1 (800) 283-4465 | https://www.hsd.state.nm.us/lookingforassistance/field_offices_1/ |
| New York | New York Medicaid | Department of Health | 1 (800) 541-2831 | https://www.health.ny.gov/health_care/medicaid/ldss.htm |
| North Carolina | North Carolina Medicaid | Division of Health Benefits | (888) 245-0179 | https://www.ncdhhs.gov/divisions/social-services/local-dss-directory |
| North Dakota | North Dakota Medicaid | Department of Human Services | (701) 328-7068 | https://www.hhs.nd.gov/human-service/zones |
| Ohio | Ohio Medicaid | Department of Medicaid | 1 (800) 324-8680 | https://jfs.ohio.gov/about/local-agencies-directory |
| Oklahoma | SoonerCare | Human Services | (888) 365-3742 | https://oklahoma.gov/okdhs/contact-us/dhsofficelocations.html |
| Oregon | Oregon Health Plan | Health Authority | (800) 273-0557 | https://www.okdhs.org/countyoffices/Pages/default.aspx |
| Pennsylvania | Medical Assistance | Department of Human Services | 1 (866) 550-4355 | https://www.dhs.pa.gov/Services/Assistance/Pages/CAO-Contact.aspx |
| Puerto Rico | Puerto Rico Medicaid | Department of Health and Human Services | (787) 765-2929 Ext. 6700 | https://medicaid.pr.gov/Home/DescripcionPrograma/ |
| Rhode Island | RI Medicaid | Executive Office of Health and Human Services | (401) 784-8100 | https://dhs.ri.gov/about-us/dhs-offices |
| South Carolina | Healthy Connections Medicaid | Department of Health and Human Services | (888) 549-0820 | https://www.scdhhs.gov/site-page/where-go-help |
| South Dakota | South Dakota Medicaid | Department of Social Services | 1 (800) 597-1603 | https://dss.sd.gov/findyourlocaloffice/ |
| Tennessee | TennCare | Department of Human Services | 1 (800) 342-3145 | https://www.tn.gov/humanservices/for-families/supplemental-nutrition-assistance-program-snap/office-locator-family-assistance.html |
| Texas | Texas Medicaid | Department of Health and Human Services | 1 (800) 335-8957 | https://www.dshs.texas.gov/regions/default.shtm |
| U.S. Virgin Islands | Virgin Islands Medicaid | Department of Human Services | (340) 715-6929 | https://www.vimmis.com/Lists/Contact%20Virgin%20Islands%20Medicaid/USVI%20Contact%20Information.aspx |
| Utah | Utah Medicaid | Department of Health and Human Services | Salt Lake City: (801) 538-6155 Other Locations: 1 (800) 662-9651 | https://jobs.utah.gov/jsp/officesearch/#/map |
| Vermont | Green Mountain Care | Department of Vermont Health Access | 1 (800) 250-8427 | https://www.healthvermont.gov/local |
| Virginia | Cover Virginia | Department of Medical Assistance Services | 1 (833) 522-5582 | https://coverva.dmas.virginia.gov/apply/find-help-in-your-area/ |
| Washington | Apple Health | Health Care Authority | 1 (800) 562-3022 | https://www.dshs.wa.gov/ALTSA/resources |
| West Virginia | West Virginia Medicaid | West Virginia Medicaid | 1 (800) 318-2596 | https://dhhr.wv.gov/pages/field-offices.aspx |
| Wisconsin | BadgerCare | Department of Health Services | 1 (800) 362-3002 | https://www.dhs.wisconsin.gov/forwardhealth/imagency/index.htm |
| Wyoming | Wyoming Medicaid | Wyoming Medicaid | (307) 777-7531 | https://health.wyo.gov/contact/ |
Common Medicaid Terms

Beneficiary
An individual who meets all the required criteria for receiving health coverage through the Medicaid program in his or her state or territory and is officially enrolled in a health care plan.
Benefits
The specific health care services and treatments that a beneficiary receives through his or her Medicaid health care plan. There are some mandatory benefits that all states and territories must provide, as well as optional additional benefits that vary throughout the country.
Centers for Medicare and Medicaid Services (CMS)
The federal agency in the Department of Health and Human Services (DHHS) that oversees the Medicaid, Medicare and State Children’s Health Insurance programs.
Coverage
A beneficiary’s right to reimbursement or payment for health care costs under Medicaid or a contract with a Medicaid-approved health care plan. Medicaid health plans outline health coverage options in member handbooks.
Copayment
A fixed fee that a beneficiary pays to a health care provider (like a doctor, hospital or specialist) in exchange for receiving treatment or services. Copayments are sometimes known as “copays.”
Cost Sharing
The term for dividing up the total cost of health care between Medicaid and the beneficiary. A copayment is an example of a type of cost share that the beneficiary pays out of pocket.
Coinsurance
The percentage of the total cost of a health care service that the beneficiary is responsible for paying out of pocket after they have paid their deductible. For example, if the total cost of services is $100 and the beneficiary’s coinsurance is 20 percent, he or she would pay $20 and the insurance company would pay the rest.
Deductible
The total amount of money a beneficiary must pay before his or her health insurance begins paying. Typically, after meeting the deductible, the beneficiary is then charged copayments for services.
Disability
A limit in a range of major life activities, including seeing, hearing, walking, thinking and working.
Dual-Eligible
A beneficiary who is eligible for both Medicaid and Medicare, as well as payment for Medicare premiums, deductibles and coinsurance.
Early and Periodic Screening, Diagnostic and Treatment (EPSDT) Services
These are mandatory services provided to all Medicaid-eligible children in each state and territory. EPSDT services include preventive health screenings for physical and mental health ailments, vision tests, hearing tests and dental exams.
Family Planning Services
Services involved in promoting healthy pregnancies while avoiding unintended pregnancies. States are allowed to define the specific family planning services covered through Medicaid.
Federal Poverty Level (FPL)
A measure of income that is determined each year by the Department of Health and Human Services. Federal poverty levels are used to determine eligibility for many government assistance programs, including Medicaid.
Federally Qualified Health Center (FQHC)
A health clinic, office or other location that provides health care services to medically underserved areas and populations. Medicaid beneficiaries can receive primary care and other ambulatory care services at community health centers and migrant health centers.
Fee-for-Service (FFS)
A method of health insurance in which the doctor or hospital is paid for providing health care services. With fee-for-service plans, either the beneficiary pays directly and submits a claim to his or her insurance company, or the provider pays on behalf of the beneficiary and files for reimbursement.
Home Health Services
Health care services or treatments that a beneficiary receives in his or her home.
Inpatient Care
Any health service or treatment that requires the beneficiary to be admitted as a patient into a hospital, skilled nursing facility or other health care setting.
Managed Care Organization (MCO)
A health insurance company that has entered into a contract with a state Medicaid agency to provide a specified package of health care benefits to Medicaid enrollees. Some states allow beneficiaries to choose their own MCO, while others assign MCOs based on a set of criteria.
Medically Necessary
A health care service that is needed to diagnose or treat an illness, injury, condition, disease or its symptoms and that meets accepted standards of medicine.
Medically Needy
Individuals who have a high amount of medical expenses and qualify for Medicaid coverage categorically, but have incomes that exceed their state or territory’s limits. Some states and territories allow these individuals to receive coverage through Medicaid.
Modified Adjusted Gross Income (MAGI)
Medicaid agencies use an applicant’s MAGI to determine if he or she qualifies for coverage based on income. MAGI includes adjusted gross income as well as untaxed foreign income, non-taxable Social Security benefits and tax-exempt interest. It does not include Supplemental Security Income (SSI).
Out-of-Pocket Costs
Health care fees and costs that are not covered or reimbursed by a health insurance company. These include copayments, coinsurance and deductibles.
Outpatient Care
A health care service or treatment in a hospital that does not require an overnight stay.
Premium
Monthly health insurance fees that beneficiaries pay to remain enrolled in a health care plan.
Prior Authorization
The requirement for a health insurance company or a government program like Medicaid to deem a service “medically necessary” before it is approved as a covered service.
Program of All-Inclusive Care for the Elderly (PACE)
Some states offer specific Medicaid-covered services to adults age 55 or older who need the level of care provided by a nursing facility. Qualifying beneficiaries receive all Medicaid-covered services through the PACE provider in which they enroll.
Qualified Medicare Beneficiary (QMB)
A Medicare beneficiary whose income or assets are too high to qualify for full Medicaid coverage as a dual eligible, but whose income is at or below 100 percent of the federal poverty level (FPL) and whose countable resources do not exceed $4000. QMBs can have Medicaid pay all of their Medicare cost-sharing requirements, including monthly premiums for Part B coverage, and all required deductibles and coinsurance.
Rural Health Clinic
A health care office or clinic located in a rural area or designated as an essential provider of primary care health services.
Supplemental Security Income (SSI)
A monthly benefit paid to individuals with low incomes and who are disabled, blind or 65 years of age or older.
Specified Low-Income Medicare Beneficiary (SLMB)
A Medicare beneficiary whose income or assets are too high to qualify for full Medicaid coverage as a dual eligible, but whose income is between 100 and 120 percent of the federal poverty level (FPL) and whose countable resources do not exceed $4000. SLMBs can have Medicaid pay their monthly premiums, but they are still responsible for paying their cost-sharing requirements.
Medicaid Benefits
Because it is partially operated by state and local governments, Medicaid benefits vary from state to state. However, there are some mandatory benefits that all states must provide to beneficiaries.
Mandatory Benefits
Mandatory benefits must be included in all state Medicaid packages. There may be copayments and other costs involved in seeking these benefits. However, any existing copayments and costs should generally be low and affordable to beneficiaries. Refer to the section called “Medicaid Cost-Sharing” for more information on copayments and costs.
The mandatory benefits are:
- Inpatient hospital visits
- Outpatient hospital visits
- Nursing facility services
- Home health services
- Physician services
- Rural health clinic services
- Early and periodic screening, diagnostic and treatment (EPSDT) services
- Federally qualified health center services
- Lab and x-ray services
- Family planning services
- Nurse midwife services
- Certified pediatric and family nurse practitioner services
- Freestanding birth center services, when licensed or otherwise recognized by the state
- Medical transportation services
- Tobacco cessation counseling services for pregnant women
- Medication assisted treatment (MAT)
- Service and item costs for beneficiaries enrolled in qualifying clinical trials
Refer to the section called “Common Medicaid Terms” for more explanation of these benefits.
Optional Additional Benefits
Optional benefits may be included in Medicaid benefits in your state, depending on your state’s policies. Check your state or territory’s benefits to determine whether any of the following benefits are included:
- Adult daycare services
- Allergy services
- Ambulatory services
- Anesthesia
- Bariatric surgery
- Breast and cervical care services
- Case management services
- Chiropractic services
- Clinic services
- Community-first choice options
- Dental services
- Denture coverage
- Dialysis
- Durable medical equipment
- Eyeglasses coverage
- Gastrointestinal services
- Gender reassignment care
- Genitourinary services
- Health homes for individuals with chronic conditions
- Hearing services
- HIV/AIDS services
- Home-delivered meals
- Hospice care
- Immunizations
- Inpatient psychiatric services for individuals under 21 years of age
- Interpreter services
- Long-term care
- Maternity care
- Mental health care
- Neurology services
- Nutritional counseling services
- Occupational therapy
- Optometry services
- Oral and maxillofacial surgery
- Orthotics
- Other approved services
- Other diagnostic, screening, preventative and rehabilitative services
- Other practitioner services
- Out-of-state care
- Peer-recovery services
- Personal care
- Physical therapy
- Podiatry services
- Postpartum care
- Prenatal care
- Prescription drug coverage
- Private duty nursing services
- Prosthetics coverage
- Radiology services
- Reconstructive surgery
- Rehabilitative services
- Respiratory care services
- School-based services
- Self-directed personal assistance services
- Services for individuals 65 years of age or older in institutions for mental diseases
- Services in intermediate care facilities for individuals with intellectual disabilities
- Skin services
- Speech, hearing and language disorder services
- State plan home and community-based services
- Transplant care
- Tuberculosis-related services
- Urgent care
- Vision care
Optional Benefits by State and Territory
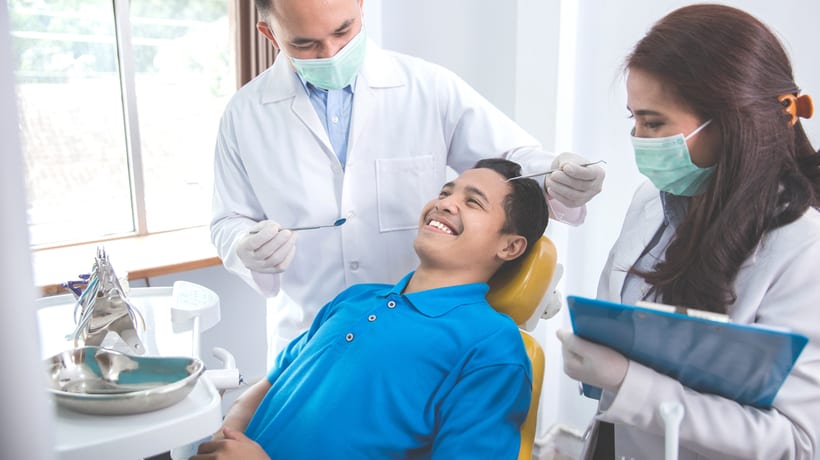
Note:
The list does not include federal mandatory benefits, which are available in all states.
Alabama
- Dental services for individuals under 21 years of age who qualify for full Medicaid coverage
- Eye care services
- Preventative health and education services
- Hearing services for individuals under 21 years of age
- Home health services
- Hospice services
- Psychiatric hospital services for children under 21 and adults over 65
- Prenatal and postpartum maternity services
- Mental health services
- Nursing home care services
- Out-of-state services
- Prescription drugs
- Renal dialysis services
- Transplant services
- Home and community-based care services
- Radiology services
- Maternity services including prenatal care
- Inpatient and outpatient hospital services when medically necessary
Alaska
- Ambulatory surgical center services
- Behavioral health services
- Inpatient psychiatric hospital services for individuals under 21 and over 65
- Residential psychiatric treatment services for individuals under 21 years of age
- Breast and cervical cancer checkups
- Chiropractic services for children
- Community first choice services
- Dental services including orthodontia for children under age 21
- Dialysis for end-stage renal disease
- Family planning services and supplies
- Hearing services
- Home and community-based waiver services
- Home health services
- Hospice services
- In-patient and outpatient hospital services including surgery when medically necessary
- Long-term care services
- Durable medical equipment and supplies
- Nutrition services for high-risk individuals under 21 years of age & pregnant women
- Personal care services
- Prescription drugs
- Podiatry services
- Prenatal and postpartum medical services
- Private duty nursing services
- School-based services, including hearing, speech-language, physical, occupational and behavioral therapy
- Physical therapy services
- Occupational therapy services
- Speech-language therapy services
- Medical transportation
Arizona
- Immunizations
- Prescription drugs
- Specialist care
- Podiatry services
- Behavioral health services
- Dialysis
- Vision Services for individuals under 21
- Dental Services for individuals under 21
- Hearing Services for individuals under 21
- Family planning services
- Pregnancy care
- Chiropractic services
Arkansas
- Adult Behavioral Health Services for Community Independence (ABHSCI)
- Applied Behavior Analysis for children with autism
- Ambulatory surgical center services
- Hearing services for individuals under 21
- Dental services for individuals under 21
- Developmental rehabilitation services for children under 3
- Chiropractic services
- Durable medical equipment
- End-stage renal disease services
- Health care independence program for medically frail people ages 19-64
- Hospice services
- Inpatient psychiatric services for individuals under 21
- Intermediate care facility services for individuals with intellectual disabilities
- Medical supplies
- Nursing facility services
- Occupational, physical and speech therapy services for individuals under 21
- Orthotic appliances
- Outpatient behavioral health services
- Personal care services
- Podiatrist services
- Prescription drug coverage
- Private duty nursing services
- Prosthetic devices
- Rehabilitative services
- Respiratory care services for individuals under 21
- School-based mental health services for individuals under 21
- Targeted case management services
- Ventilator equipment
- Vision services
California
- Abortion and family planning services and supplies
- Acupuncture
- Ambulance transportation
- Emergency room services
- Bariatric surgery
- Podiatry services
- Chiropractic services
- Allergy care
- Treatment therapies (chemotherapy, radiation therapy, etc.)
- Dialysis
- Outpatient mental health services (including specialty)
- Substance use disorder services
- Inpatient specialty mental health services
- Prescription drug services
- Physical and occupational therapy services
- Speech therapy/audiology
- Durable medical equipment services
- Medical supplies, equipment and appliances
- Hearing aids
- Dental services
- Diabetic services
- Gender reassignment surgery
- Vision services
- Personal care services and other long-term services and supports
- Prenatal, delivery and postpartum care including a certified nurse, midwife and birthing centers
- Preventive services and vaccines
- Behavioral health treatment for individuals under 21
- Radiology services
- Reconstructive surgery (non-cosmetic)
- Kidney transplants for individuals under 21
Colorado
- Vision services
- Dental services
- Hospice services
- Private nursing services
- Mental and behavioral health services
- Inpatient mental health services
- Outpatient mental health services
- Prescription drug services
- Durable medical equipment services
- Physical and occupational therapy services
- Speech therapy services
- Transplant services
- Immunizations
- Hearing services
- Podiatry services
- Breast reconstruction surgery for individuals with breast disease diagnosis and related surgery in prior 5 years
- Radiation therapy and chemotherapy services
- Pregnancy services, including coverage for newborns up to age one
- Telemedicine
- Ambulance services and other medical transportation
- Emergency room visits and urgent care facilities
- Substance abuse services
- Private duty nursing up to 16 hours a day for adults, unlimited for children under 21
- Lab and radiology tests
- Allergy services
- Surgical sterilization for individuals over 21
- Contraceptives
Connecticut
- Preventive care
- Women’s health care and family planning services
- Maternity care
- Long-term services and supports
- Physical and occupational therapy services
- Speech therapy services
- Hearing services (audiology and hearing aids)
- Physical rehabilitation
- Dialysis
- Vision services
- Durable medical equipment (DME) services
- Orthotic and prosthetic devices
- Hospice services
- Dental services
- Behavioral health services
- Prescription drug services
- Home health care
- For Husky A, C and D members
- Non-emergency medical transportation
- Smoking cessation
- EPSDT
Delaware
- Drug and alcohol abuse services
- Speech therapy services
- Hearing services
- Immunizations
- Physical therapy services
- Eye exams but not eyeglasses
- Prescription drug services
- Assistive technology
- Mental health and substance abuse services including residential
- Case management and coordination
- Hospice services
- Dental services but not dentures
- Telemedicine
- Rural health clinic and federally qualified health center services
- Ambulatory services for pregnant women and individuals under 18
- Lab and x-ray services
- Nursing facility services other than mental health facilities for individuals 21 and older
- Family planning services but not fertility-related services
- Podiatry
- Tobacco cessation counseling
- School-based services
- Chiropractic services
- Home health services and supplies and equipment for home use
- Licensed midwife services
- Private duty nursing
- Prosthetic devices
- Behavioral services to treat autism in children under 21
- Lactation counseling
- Day health and rehabilitation for individuals with mental retardation disabilities
- Medical transportation
District of Columbia
- Eyecare
- Ambulatory surgical center
- Dental services and related treatment
- Dialysis services
- Durable medical equipment
- Hospice services
- Laboratory services including radiology
- Medical supplies
- Mental health services
- Home and Community-Based Services (HCBS)
- Transplants
Florida
- Allergy services
- Ambulatory surgical centers
- Anesthesia
- Assistive care
- Behavioral analysis and services
- Birth Center and midwife services
- Cardiovascular services
- Chiropractic services
- Community behavioral health services
- County Health Department (CHD) Services
- Dental services, oral and maxillofacial surgery
- Dialysis
- Durable medical equipment (DME) and supplies
- Family planning waiver services
- Gastrointestinal services
- Genitourinary services
- Hearing services
- Home health services
- Hospice services
- Integumentary Services
- Hospital: inpatient, outpatient, both medical and behavioral
- Intermediate Care Facility for Individuals with Intellectual Disabilities (ICF/IID) services
- Medical Foster Care (MFC) services
- Neurology
- Nursing facility
- Oral and maxillofacial surgery
- Orthopedic services
- Pain management
- Podiatry
- Prescription drugs
- Prescribed Pediatric Extended Care (PPEC) services
- Reproductive services
- Respiratory services
- School-based services programs
- Specialized therapeutic foster care
- Targeted case management – mental health
- Therapy (Occupational, physical, respiratory, speech-language)
- Transplant services
- Medical transportation, emergency and non-emergency
- Vision services and visual aid
Georgia
- Prescription drugs
- Behavioral health services including inpatient psychiatric care for individuals under 21
- Preventive dental care for children
- Kidney transplants; limited liver transplants
- Inpatient hospital services up to 30 days, medical and behavioral
- MRIs
- Nursing facility swing-bed services
- Dental services
- Home health nursing, aide and medical supplies and equipment
- Outpatient dialysis
- One series of birthing and parenting classes per year for pregnant women
- Tobacco cessation counseling for pregnant women
- Family planning services
- Certain emergency dental care procedures for adults
- Medical equipment and supplies prescribed by a doctor and used in the home
- Exams and immunizations for children
- Hospice care
- Vision services for children (limited service for adults)
- Hearing services for children
- Mental health clinic services
- Case management
- Mental Retardation Waiver Program
- Community Care Services Program
- Independent Care Waiver Program
- Orthotics and prosthetics
- Podiatry services
- Speech, physical and occupational therapy
- Psychological services for individuals under 21
- Dialysis and services for end-stage renal disease
- Durable medical equipment
Hawaii
- Adult daycare
- Nursing home and assisted living services
- Non-medical transportation for seniors
- Respite care
- Skilled nursing
- Behavioral health services
- Home delivered meals and home maintenance for individuals who qualify for long-term services
- Community care services
- Dental care
- Dialysis
- Durable medical equipment (DME)
- Habilitation services
- Hospice services
- Intellectual and developmental disease (I/DD) services
- Immunizations
- Long-Term Services and Supports (LTSS)
- Organ and tissue transplant services
- Outpatient hospital procedures including surgeries at ambulatory surgery centers and sleep laboratory services
- Nutritional counseling
- Smoking cessations
- Urgent care
- Vision and hearing services
- Pregnancy-related services
- Prescription drugs
- Rehabilitation services
- Termination of pregnancy services
Idaho
- Counseling and mental health services
- Mental health counseling and services
- Dental services
- Durable medical equipment (DME) and medical supplies
- Emergency and non-emergency medical transportation
- Home health care with a doctor’s prescription
- Hospice care
- Chiropractic services
- Nutrition services
- Immunizations
- Pregnancy services
- Prescription drugs
- Prosthetics and orthotics
- Smoking cessation
- Substance abuse treatment services
- Vision services
- Weight loss services
- X-rays
Illinois
- Dental services
- Maternity care
- Surgery
- Prescription drugs
- Mental health treatment
- Substance abuse treatment
- Medical supplies and equipment
- Nursing home care
- Physical, speech and occupational therapy
- Eyeglasses and optometrist services
- Hearing services
- Podiatry services
- Chiropractic services
- Intermediate care for people who are developmentally disabled
- Dialysis services
- Hospice care
- Respiratory equipment and other medical supplies
Indiana
- Prescription and over-the-counter drugs
- Mental health care
- Substance abuse services
- Medical supplies and equipment
- Dental care
- Vision care
- Physical, occupational and speech therapy
- Hospice care
- Podiatry
- Chiropractic care
- Lab and x-ray services
- Home health care
- Nursing facility services
- Emergency and non-emergency transportation
Iowa
- Ambulance and non-emergency medical transportation
- Ambulatory surgical centers
- Birth control and family planning
- Chiropractic services
- Eye exams and eyeglasses
- Habilitation services
- Home health care
- Hospice care
- Hospital and urgent care
- Prescription drugs and over the counter drugs
- Podiatry and orthopedic shoes
- Occupational, physical and speech therapy
- Tobbaco cessation services
- Women’s health services including maternity care and birth centers
- Substance abuse services
- Mental health care
- Dental care
- Preventive health services
Kansas
- Vaccines
- Behavioral health services
- Prescription drugs
- Eye care visits
- Dental care for children (some preventive procedures for adults)
- Transportation to medical appointments
- Nursing facility services
- Heart and lung transplants for adults
- Weight loss surgery
Enrollees will have additional benefits based on the health plan they choose: https://www.kancare.ks.gov/consumers/choosing-a-plan
Kentucky
- Intermediate care facilities for people with intellectual disabilities
- Behavioral health and substance abuse services
- Prenatal care
- Breast and cervical cancer treatment
- Tobacco cessation
- Medical transportation
- Dental services
- Vision services
- Prescription drugs
Specific information about covered services can be found by contacting one of the managed care organizations (MCOs) that provide Medicaid in Kentucky. Contact information can be found below:
- Aetna Better Health of KY – (855) 300-5528
- Anthem Blue Cross Blue Shield – (855) 690-7784
- Humana Health Plan – (800) 444-9137
- Passport Health Plan – (800) 578-0603
- Wellcare of Kentucky – (877) 389-9457
Louisiana
- Behavioral health services including psychiatric hospital care
- Chemotherapy
- Chiropractic care
- Dental and orthodontic care
- Dentures for adults
- Durable medical equipment (DME)
- Audiology and hearing aids
- Hemodialysis services
- Hearing services and hearing aids
- Hospice care
- Immunizations
- Long-term personal care services
- Occupational, physical and speech therapy
- Pediatric Day Health Care (PDHC)
- Program for All-Inclusive Care for the Elderly (PACE)
- Prescription drugs
- Podiatry services
- Prenatal care and midwife services
- Psychiatric care and behavioral health for adults
- Rehabilitation services
- STD clinics
- Vision care
Maine
Some of Maine’s covered services require prior authorization. Your doctor will get approval from the MaineCare program.
- Preventive services (immunizations, pap smears, mammograms, prostate exams, eye exams)
- Behavioral and mental health services
- Chiropractic services
- Substance use disorder treatment
- Durable medical equipment (DME) and supplies including oxygen and oxygen equipment services
- Prescriptions
- Hearing aids and hearing services
- Eye care and vision services
- Podiatry
- Rehabilitative services
- Dental services
- Psychiatric inpatient treatment
- Dialysis
- Hospice services
- Intermediate care facility for people with intellectual disabilities
- Occupational, physical and speech therapy
Covered services depend on the member’s specific benefit package. For more benefits information, call MaineCare Member Services at 1 (800) 977-6740 or 711 (TTY).
Maryland
- Ambulatory surgical services
- Ambulatory and wheelchair van services
- Biomarker testing (cancer)
- Dental services for all ages and dentures for beneficiaries under 21 years of age
- Diabetes care
- Eyeglasses for beneficiaries under 21 years of age
- Family planning services and supplies
- Hearing aids for beneficiaries under 21 years of age
- Home health care
- Hospice care
- Dialysis services
- Medical daycare services
- Medical equipment and supplies
- Nursing facilities
- Medical transportation
- Mental health services
- Oxygen and other respiratory services
- Personal care services
- Pregnancy care
- Prescription drugs
- Physical therapy
- Podiatry services
- School-based medical care for children
- Statewide Evaluation and Planning Services (STEPS) through local health departments
- Substance abuse treatment services
- Targeted case management for HIV-infected beneficiaries and other populations
- Vision care every two years
Massachusetts
- Therapies
- Dental services
- Prescription drugs including birth control drugs
- Vision care and eyeglasses
- Hearing aids
- Medical equipment and supplies
- Adult day health and foster care
- Mental health and addiction services
- Long-term care services and support at home or in a facility
- Smoking cessation services
- Medical transportation (requires pre-authorization)
- Occupational, physical and speech therapy
- Gender affirming care including surgery
Michigan
- Chiropractic care
- Dental care
- Family planning
- Hearing and speech services
- Home health care
- Hospice care
- Medical supplies
- Prescription drugs
- Mental health services
- Nursing home care
- Private duty nursing
- Personal care services
- Physical and occupational therapy
- Podiatry
- Pregnancy and postpartum care
- Immunizations
- Substance abuse treatment
- Surgery
- Vision care
Minnesota
- Alcohol and drug treatment
- Birth center services
- Chiropractic care
- Dental care
- Eyeglasses
- Family planning services
- Hearing aids
- Hospice care
- Immunizations
- Interpreter services
- Medical equipment and supplies
- Medical transportation
- Mental health care
- Intermediate care facilities for people with developmental disabilities
- Prescriptions and medication therapy management
- Rehabilitative therapy
- Urgent care
Mississippi
- Ambulatory surgical center
- Assisted living facility
- Autism spectrum disorder services
- Chiropractic care
- Community homes and immediate care facilities for people with intellectual disabilities
- Dental care, oral surgery and orthodontics
- Dialysis services
- Durable medical equipment (DME) and medical supplies
- Vision and eyeglasses
- Hearing aids and services
- Hospice services
- Long-term care
- Medical supplies
- Occupational, physical and speech therapy
- Organ transplants
- Podiatry services
- Prescription drugs
- Psychiatric care and mental health services including inpatient psychiatric hospitalization
- School-based services
- Vaccines
Missouri
- Ambulatory surgical centers and birthing centers
- Audiology services and hearing aids
- Asthma services for individuals under 21
- Behavioral health and substance use services including emergency
- Complementary health and alternative therapy for chronic pain (adults 21 and over)
- Case management for pregnant women
- Community psychiatric rehabilitation services
- Comprehensive substance treatment and rehabilitation (C-STAR)
- Dental services
- Diabetes prevention program
- Comprehensive data rehab for serious head injury
- Durable medical equipment (DME) and some prosthetic/orthotic devices
- Family planning services
- Hearing aids and related services
- Hospice care
- Non-emergency medical transportation
- Personal care and adult day health care services
- Podiatry services
- Prescription drugs
- Private duty nursing for childer under 21
- Speech, occupational and physical therapy for children under 21
- Orthodontics for children under 21
- Rehabilitative services
- Transplant services
- Vision services and eyeglasses
Montana
- Dental care
- Audiology and hearing aids
- Family planning services
- Maternity and newborn care
- Mental health and substance abuse services
- Prescription drugs
- Rehabilitative services and supplies
- School-based health services
- Speech therapy
- Medical transportation
- Substance abuse services
- Vision services every two years
Nebraska
- Chiropractic services
- Dental care
- Durable medical equipment (DME), orthotics, prosthetics and medical supplies
- Family planning services
- Hearing aids
- Hospice care
- Home health agency services
- Intermediate Care Facilities for Persons with Intellectual Disabilities (ICF/DD)
- Medical transportation services
- Mental health and substance abuse services
- Nurse midwife services
- Nursing facility
- Private duty nursing services
- Occupational, speech, physical and audiological therapy
- Personal assistance services
- Podiatry
- Prescription drugs
- Private-duty nursing
- Program of All-Inclusive Care for the Elderly (PACE)
- Mammograms
- Medically necessary psychiatric and substance abuse services for adults
- Vision care every two years
Nevada
- Ambulance/transportation
- Birth control/family planning
- Dental care
- Disposable medical supplies
- Durable medical equipment (DME)
- Eye exams and glasses
- Hearing tests
- Home health care
- Hospice care
- Immunizations
- Maternity care
- Mental health services
- Midwife services
- Nursing home services
- Occupational and physical therapy
- Orthotics and prosthetics
- Over-the-counter drugs with a prescription
- Personal care services
- Private duty nursing
- Prescription drugs
- Smoking cessation products
- Specialist visits
- Speech and hearing services
- Substance abuse services
New Hampshire
- Adult medical daycare
- Dental care
- Durable medical equipment (DME) and medical supplies
- Extended services for pregnant women
- Hearing services
- Hospice services
- Interpreter services
- Newborn home visits
- Nursing facility
- Home health
- Medical transportation
- Interpreter
- Certified midwife
- Family planning
- Personal care attendant services
- Physical, occupational and speech therapy
- Podiatry
- Prescription drugs
- Private duty nursing
- Psychotherapy
- Vision care
New Jersey
- Chiropractic services
- Dental care
- Durable medical equipment (DME)
- Family services and supplies
- Hearing aid services
- Hospice care
- Inpatient psychiatric care for individuals under 21 and over 65
- Intermediate care facilities for people with intellectual disabilities
- Licensed practitioner services
- Optical appliances
- Personal care services
- Physical, occupational and speech therapy
- Podiatry
- Prescription drugs
- Private duty nursing
- Prosthetics and orthotics
- Psychological care including inpatient psychiatric care for individuals u. der 21 and over65
- Intermediate care facilities for the mentally retarded
- Vision care
New Mexico
- Adult daycare
- Preventive services
- Behavioral health care
- Long-term care
- Medical transportation
- Vision services
- Specialist services
Specific benefits may vary depending on the plan beneficiaries choose. Applicants are able to choose among four Medicaid plans: BlueCross BlueShield, Presbyterian, Western Sky or United Healthcare.
New York
- Dental care
- Medical supplies and equipment
- Mental health services
- Home health care including personal care aides
- Adult daycare
- Physical, occupational and speech therapy
- Durable medical equipment
- Family planning services
- Medicaid Health Homes comprehensive care management
- Nursing home services
- Preventive services
- Personal care services
- Prenatal care
- Prescription drugs
- Smoking cessation agent
- Vision care and eyeglasses
North Carolina
- Ambulatory surgical centers
- Dental and orthodontic services for children
- Hearing services
- Medical equipment
- Mental and behavioral health care
- Intellectual/developmental care
- HIV case management
- Family planning services
- Infant toddler program for children up to age 3 with developmental delays
- Home health services
- Hospice
- Nursing facilities
- Private duty nursing
- Chiropractic services
- Durable medical equipment
- Dialysis
- Well-woman services (OB/Gyn)
- Physical, occupational, speech, respiratory and audiology therapy
- Radiology
- Orthotics and prosthetics
- Prescription drugs
- Podiatry
- Personal care services
- Specialized therapy
- Vision services and aids
North Dakota
- Chiropractic care
- Dental care
- Durable medical equipment (DME) and supplies
- Hospice care
- Mental health care
- Nursing facility
- Home health care
- Family planning
- Prescription drugs
- Podiatry
- Speech, physical and occupational therapy
- Sterilization
- Vision care
- Medical transportation
Ohio
- Alcohol and drug addiction services
- Ambulatory surgical centers
- Audiology services
- Chiropractic services
- Dental care
- Medical equipment
- Medical transportation emergency and non-emergency
- Mental health care
- Physical, speech and occupational therapy
- Podiatry
- Pregnancy care
- Prescription drugs
- Preventive health services
- Private duty nursing
- Vision care including surgical
Oklahoma
- Ambulatory surgical centers
- Behavioral health care including inpatient care for individuals 65 and older
- Outpatient substance abuse services
- Case management services
- Chemotherapy and radiation therapy
- Dental care
- Dentures for adults residing in nursing facilities
- Dialysis
- Durable medical equipment (DME) and supplies
- Family planning services and supplies
- Hemophilia care
- Home health services
- Intermediate Care Facilities for Individuals with Intellectual Disabilities (ICF/IID)
- Maternity care
- Mental health and substance abuse services
- Nutritional Services
- Maternity and pregnancy services
- Personal care services
- Podiatry services
- Prescription drugs and insulin
- Tuberculosis services
- Tobacco cessation services
- Transplants with pre-authorization
- Ultrasound benefits
Additional services for children include the following:
- Hearing aids
- Immunizations
- Incontinence supplies for certain children
- Optometric or optical services, including eyeglasses
- Orthodontics
- Physical and occupational therapy
- Private duty nursing
- Speech, hearing and language disorder services
- Other medically necessary services
Oregon
- Chemical dependency care
- Dental care and dentures
- Hearing aids and exams
- Home health care
- Hospice care
- Immunizations and vaccinations
- Labor, delivery and postpartum maternity care
- Medical equipment and supplies
- Medical transportation
- Mental health care services
- Physical, occupational and speech therapy
- Prescription drugs
- Private duty nursing
- Vision care services for pregnant women and children under 21, eyeglasses for pregnant women and adults with a qualifying medical condition
Pennsylvania
- Behavioral health services
- Chiropractic services
- Dental and orthodontic care
- Dialysis
- Durable medical equipment (DME)
- Medical Supplies
- Hospice care
- Maternity care
- Mental health and substance abuse services
- Podiatry services
- Prescription drugs
- Prosthetics and orthotics
- Specialist care
- Substance abuse services
- Tobacco cessation services
- Vision care
Rhode Island
- Dental care
- Durable medical equipment (DME)
- HIV/AIDS services
- Home stabilization services
- Home health care
- Assisted living facilities
- Nursing homes
- Hospice care
- Interpreter services
- Long-term care
- Peer recovery support services
- Podiatry
- Prescription drugs
- Rehabilitative services
- Vision care
South Carolina
- Alcohol and drug abuse services
- Adult daycare services
- Ambulatory surgical center
- Audiology services
- Behavioral health services
- Chiropractic services
- Durable medical equipment
- Eyeglasses and vision care
- Autism spectrum disorder services
- Dental services
- Family planning
- Home- and community-based long-term care services
- Nursing facilities
- Hospice care
- Incontinence supplies
- Nutritional supplement services
- Occupational, physical and speech therapy
- Prescription drugs
- Private duty nursing
- Psychiatric care and behavioral health services
- Rehabilitative therapy services
- School-based rehabilitative therapy
South Dakota
- Chiropractic care
- Dental care
- Diabetes education
- Dietician and nutritionist services
- Durable medical equipment (DME) and medical supplies
- Chiropractic care
- Dental care
- Diabetes education
- Dietician and nutritionist services
- Durable medical equipment (DME) and medical supplies
- Family planning and testing for STDs
- Hospice care
- Home healthcare
- Immunizations
- Medical transportation
- Mental health care
- Nursing home services
- Personal care services
- Physical, speech, occupational and audiology therapy
- Podiatry
- Pregnancy coverage
- Psychiatry / psychology
- Prescription drugs
- Same-day surgery centers
- School district services
- Substance abuse services
- Urgent care facilities
- Vision care and eyeglasses
Tennessee
- Behavioral health services
- Chiropractic services
- Dental services
- Dialysis
- Durable medical equipment (DME) and medical supplies
- Hospice care
- Mental health services
- Occupational, physical and speech therapy
- Organ transplants
- Prescription drugs
- Private duty nursing
- Psychiatric inpatient, residential and rehabilitative services
- Reconstructive breast surgery
- Substance abuse services
- Vision care and one pair of glasses or contacts following cataract surgery
Texas
STAR – Medicaid for children aged 18 or younger, pregnant women and families
- Breast and cervical cancer services
- Behavioral health services
- Hearing services
- Mental health care services
- Prescription drugs and vaccines
- Specialist services
- Vision care
Families are not covered unless they are caring for a child 17 or younger who is receiving Medicaid and who meet the income requirements.
STAR Plus – Medicaid for individuals with disabilities or older than 65 years of age
- Adaptive aids
- Adult foster care services
- Assisted living
- Home meal delivery and home health care
- Intermediate care facilities for individuals with an intellectual disability
- Long-term care including nursing facilities
- Medical supplies
- Minor home safety modifications
- Occupational, physical and speech therapy
- Personal care services
- Respite care
- Transitional assistance services
Utah
- Birth control
- Case management
- Chiropractic care
- Dental care
- Home health care
- Hospice care
- Individual and group therapy
- Maternity and midwife services
- Medical supplies
- Mental health medication management
- Mental health evaluations
- Mental health services
- Personal care services
- Physical and occupational therapy
- Podiatry
- Prescription and over-the-counter drugs
- Psycho-educational services
- Psychosocial rehabilitative services
- Psychological testing
- Respite care
- Specialist care
- Speech and hearing assistance
- Substance abuse services
- Tobacco cessation services
- Vision care
Vermont
- Chiropractic care
- Community mental health centers
- Dental care
- Diabetic supplies
- Eye exams but not eyeglasses
- Gynecological services
- Hearing aids
- home health aide and nursing
- Hospice care
- Immunizations
- Medical equipment and supplies
- Maxillofacial surgery
- Mental health counseling
- Midwife services
- Naturopaths
- Nutrition therapy
- Occupational, physical and speech/language therapy
- Ophthalmologist
- Organ transplants
- Podiatry
- Prescription and over-the-counter drugs
- Prosthetics
- Psychiatric and psychological care including psychiatric hospital care
- Respiratory therapy
- Specialist services
- Substance abuse treatment
- Medical transportation
Virginia
- Addiction and Recovery Treatment Services (ARTS)
- Behavioral health services
- Dental care, is comprehensive for individu als under age 21 and limited to medically necessary for adults
- Dialysis for end-stage renal disease
- Durable medical equipment (DME) and supplies
- Eye examinations
- Eyeglasses for members younger than 21 years of age
- Family planning services and birth control
- Glucose test strips
- Home health visits
- Long-term services and support
- Nursing facilities
- Organ transplants
- Personal care
- Physical, occupational and speech therapy
- Podiatry
- Program of All-Inclusive Care for the Elderly (PACE)
- Prenatal and maternity services
- Prescription drugs
- Prosthetic devices
- Psychiatric or psychological care including inpatient psychiatric hospital services for individuals under age 21 or age 65 and older; inpatient psychiatric services for patients age 22-64 in the psychiatric wing of an acute care hospital
- School health services
- Substance abuse treatment
Washington
- Alcohol and addiction services
- Autism and applied behavioral analysis therapy
- Breast, cervical and colon health program
- Dental care
- Family planning
- Gender-affirming treatments and surgery
- Home health care
- Interpreter services
- Long-term services and supports
- Medically intensive children’s program (MICP)
- Maternity and newborn care
- Mental health services
- Non-emergency medical transportation
- Prescription drugs
- Vision screening for children
West Virginia
- Cardiac rehabilitation
- Chiropractic care
- Dental care: comprehensive for individuals age 21 and younger, limited for adults
- Diabetes education
- Durable medical equipment (DME)
- Family planning services and supplies
- Home health care
- Hospice care
- Maternity care
- Non-emergency transportation
- Nursing home
- Nutritional counseling
- Orthotics and prosthetics
- Personal care services
- Physical, occupational and speech therapy
- Podiatry
- Prescription drugs
- Psychiatric care
- Pulmonary rehabilitation
- Specialty care
- Tobacco cessation
- X-rays
Wisconsin
- Ambulatory surgery centers
- Case management services
- Chiropractic services
- Dental services
- Dialysis
- Durable medical equipment and disposable supplies
- Eyecare, eyeglasses and exams
- Family planning services
- Hearing services
- Home health care
- Hospice care
- Intermediate care facility (ICF) services
- Medical supplies and equipment
- Medical transportation
- Mental health care and substance abuse services
- Nursing home services
- Psychosocial rehabilitative services
- Personal care services
- Physical and occupational therapy
- Podiatry services
- Prenatal care coordination for women with high-risk pregnancies
- Prescription and over-the-counter drugs
- Respiratory care services for ventilator-dependent members
- Speech, hearing, and language disorder services
- Substance abuse services
- Tuberculosis (TB) services
- Vision care services including eyeglasses
Wyoming
- Ambulatory surgical center services
- Care management entity as an alternative to a psychiatric residential treatment facility for individuals age 21 and younger
- Chiropractic services
- Dental services for individuals age 21 and younger, limited orthodontics for children ages 6-18; for adults over age 21, preventative and emergency dental services
- Developmental center services for children age 5 and younger
- Developmental disability comprehensive services
- Dietician services
- Durable medical equipment
- Dialysis
- Family planning services
- Hearing services including hearing aids
- Home health services
- Intermediate care facility for the intellectually disabled
- Interpretation services
- Mental health and substance abuse services
- Nurse midwife services
- Nursing facility services
- Organ transplant services
- Prosthetics and orthotics
- Psychiatric hospital services for individuals over the age of 21
- Speech, occupational and physical therapy
- Medical transportation
- Vision services including eyeglasses for individuals under the age of 21
U.S. Territories:
American Samoa
American Samoa is exempt from covering mandatory benefits. It provides 10 of the 17 mandatory benefits. Examples of mandatory programs it does not offer include:
- Nursing facility services
- Nurse midwife services
- Freestanding birth center services
Optional benefits offered by American Samoa Medicaid include:
- Dental care
- Psychologist Services
- Prescription drugs
- Federally qualified health center (FQHC) benefits
- Early and periodic screening, diagnostic and treatment (EPSDT) services for any members younger than 21 years of age
- Chiropractic services
- Dental services including dentures
- Eyeglasses
- Home health services
- Hospice services
- Inpatient hospital and nursing facility services for individuals age 65 or older in institutions for mental diseases
- Intermediate care facility services for individuals with intellectual disabilities
- Occupational, physical and speech therapy
- Optometry services
- Personal care services
- Primary care case management services
- Private duty nursing services
- Prosthetic devices
- Respiratory care for ventilator-dependent individuals
- Services furnished in a religious nonmedical health care institution
Guam
Guam provides all mandatory benefits. Optional benefits in Guam include:
- Dental care
- Prescription drug coverage
- Chiropractic services
- Dental services including dentures
- Eyeglasses
- Home health services
- Hospice services
- Inpatient hospital and nursing facility services for individuals age 65 or older in institutions for mental diseases
- Intermediate care facility services for individuals with intellectual disabilities
- Occupational, physical and speech therapy
- Optometry services
- Personal care services
- Primary care case management services
- Private duty nursing services
- Prosthetic devices
- Respiratory care for ventilator-dependent individuals
- Services furnished in a religious nonmedical health care institution
Commonwealth of Northern Mariana Islands
The Commonwealth of Northern Mariana Islands Medicaid program covers all mandatory benefits except freestanding birth center services. It also offers the following benefits:
- Clinic services
- Dental care and dentures
- Chiropractic services
- Dental services including dentures
- Eyeglasses
- Home health services
- Hospice services
- Inpatient hospital and nursing facility services for individuals age 65 or older in institutions for mental diseases
- Intermediate care facility services for individuals with intellectual disabilities
- Occupational, physical and speech therapy
- Optometry services
- Personal care services
- Prescription drugs
- Medical supplies
- Physical and occupational therapy
- Primary care case management services
- Prescription drugs
- Private duty nursing
- Respiratory care for ventilator-dependent individuals
- Prosthetics
- Rehabilitative Services
- Speech, hearing and language disorder services
- Services furnished in a religious nonmedical health care institution
- Targeted case management services
- Tuberculosis-related services
Puerto Rico
Comprehensive information about covered services is not readily available. To learn about all services offered, contact the Department of Health at (787) 765-2929 ext. 6700.
Puerto Rico is exempt from covering mandatory benefits. It provides 10 of the 17 mandatory benefits. Examples of mandatory programs it does not offer include:
- Nursing facility services
- Non-emergency medical transportation
- Emergency medical services for non-citizens
Optional benefits offered by Puerto Rico Medicaid include:
- Dental care
and - Prescription drugs.
- Chiropractic services
- Dental services including dentures
- Eyeglasses and optometry services
- Home health services
- Hospice services
- Inpatient hospital and nursing facility services for individuals age 65 or older in institutions for mental diseases
- Intermediate care facility services for individuals with intellectual disabilities
- Occupational, physical and speech therapy
- Optometry services
- Personal care services
- Primary care case management services
- Private duty nursing services
- Prosthetic devices
- Respiratory care for ventilator-dependent individuals
- Services furnished in a religious nonmedical health care institution
U.S. Virgin Islands
Comprehensive information about covered services is not readily available. To learn about all services offered, contact the Department of Human Services (DHS) at the following phone numbers:
- St. Thomas: (340) 774-0930
- St. Croix: (340) 718-2980
- St. John: (340) 776-6334
The U.S. Virgin Islands does not cover two of the mandatory benefits: rural health clinics and freestanding birth centers. Optional benefits include:
- Dental services
and - Prescription drugs
- Chiropractic services
- Dental services including dentures
- Eyeglasses and optometry services
- Home health services
- Hospice services
- Inpatient hospital and nursing facility services for individuals age 65 or older in institutions for mental diseases
- Intermediate care facility services for individuals with intellectual disabilities
- Occupational, physical and speech therapy
- Optometry services
- Personal care services, primary care case management services
- Private duty nursing services
- Prosthetic devices
- Respiratory care for ventilator-dependent individuals
- Services furnished in a religious nonmedical health care institution
Services Not Covered by Medicaid
Some services are not covered by Medicaid at all. For these services, individuals must seek alternative sources of funding or pay out of pocket to seek them.
If your state’s Medicaid plan does not have a particular service listed, you should assume it is not included in your benefits. However, in some cases, there may be exceptions to the list depending on an individual’s medical history, proposed treatment plan, doctor and state.
The best way to find out if you can get coverage for a service not included in your state’s standard benefits is to contact your state’s Medicaid office. Refer to the “Medicaid Contact Information By State and Territory” section to learn who you can reach out to about unlisted services.
Medicaid Expansion
Prior to the year 2010, states set different Medicaid eligibility requirements for different groups, and generally excluded low-income adults with no children or disabilities.
In 2010, the Affordable Care Act (ACA) was signed by President Barack Obama. As part of the ACA’s effort to expand health insurance coverage nationwide, states were required to expand Medicaid coverage to include all individuals whose income equaled 138 percent of the Federal Poverty Level or lower.
However, a 2012 Supreme Court ruling determined that states had the option to choose whether or not to expand Medicaid coverage to meet this new requirement. Some states have chosen to expand coverage, and some states have chosen not to expand coverage.
As of 2024, 41 states (including the District of Columbia) have adopted the Medicaid expansion and 10 have not. Your state’s choice to expand or not expand coverage can impact whether or not you qualify for Medicaid.
States That Have Expanded Medicaid Coverage
The following states have adopted expanded Medicaid income eligibility requirements under the Affordable Care Act:
- Alaska
- Arizona
- Arkansas
- California
- Colorado
- Connecticut
- Delaware
- District of Columbia
- Hawaii
- Idaho
- Illinois
- Indiana
- Iowa
- Kentucky
- Louisiana
- Maine
- Maryland
- Massachusetts
- Michigan
- Minnesota
- Missouri
- Montana
- Nebraska
- Nevada
- New Hampshire
- New Jersey
- New Mexico
- New York
- North Carolina
- North Dakota
- Ohio
- Oklahoma
- Oregon
- Pennsylvania
- Rhode Island
- South Dakota
- Utah
- Vermont
- Virginia
- Washington
- West Virginia
States That Have Not Expanded Medicaid Coverage
The following states have not adopted expanded Medicaid eligibility requirements under the Affordable Care Act:
- Alabama
- Florida
- Georgia
- Kansas
- Mississippi
- South Carolina
- Tennessee
- Texas
- Wisconsin
- Wyoming
For states that have not expanded the requirement, you must check the state’s individual eligibility requirements to determine if you qualify for Medicaid. Learn more about eligibility requirements by location in the section called “Medicaid Eligibility By State and Territory”.
What to Do if Your Location Has Not Expanded Medicaid
If your state has not expanded Medicaid requirements, you may still have options for obtaining health insurance or financial assistance for medical coverage.
Check the Marketplace
Even if you can not get coverage through Medicaid, you might be eligible for a plan through the Health Insurance Marketplace. This can be costly since you will have to pay higher premiums and more out-of-pocket expenses. However, if you have serious medical needs but do not qualify for Medicaid and cannot get health insurance through work, the Marketplace may be the best option. For information on the marketplace, go to https://www.healthcare.gov/.
If your income is between 100 and 400 percent of the Federal Poverty Level, you can get a premium tax credit that you can put toward a plan from the Marketplace. This tax credit allows you to lower the monthly cost of your premium payments to help make them more affordable. For more information on tax credits, go to https://www.irs.gov/affordable-care-act.
Reapply If Your Circumstances Change
Even if you are not eligible for Medicaid coverage when you initially apply, you may be able to receive coverage if your disability status, income or family status changes. You are allowed to reapply for Medicaid coverage if you believe your current circumstances merit coverage through the program.
Consider Relocating
If your medical expenses are costly and you cannot receive Medicaid in your current state, it may make sense to relocate to a state with expanded Medicaid coverage. If you have the ability to relocate to a state where you can earn the same or similar income and receive Medicaid assistance, you should calculate the potential costs and benefits and determine if moving is the right choice for you.
Medicaid Eligibility by State and Territory
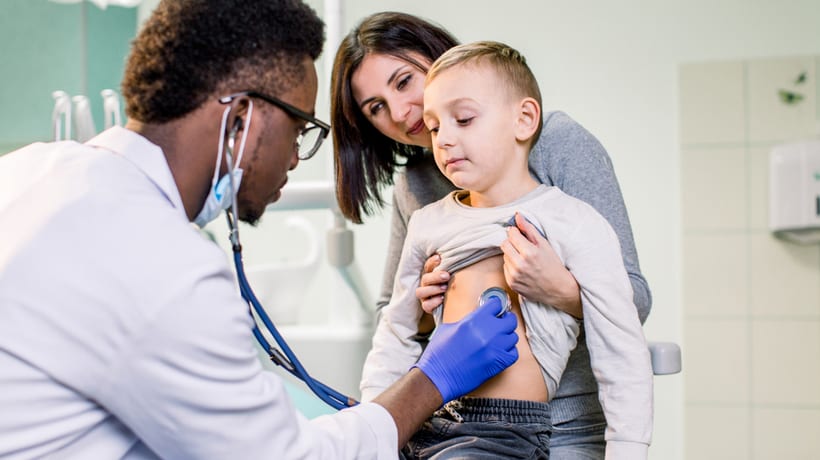
While states that have elected to expand Medicaid generally have the same eligibility requirements, states that have not done so may have a variety of different prerequisites to qualify. Check the requirements in your state below to see if you are eligible for Medicaid benefits.
Understanding Common Eligibility Requirements
Most states require individuals to earn somewhere below 138 percent of the FPL to qualify for Medicaid.
The 2026 FPL chart for the 48 contiguous states and Washington, D.C. is as follows:
| Household Size | Annual Income Limit |
| Individuals | $15,960 |
| Family of 2 | $21,640 |
| Family of 3 | $27,320 |
| Family of 4 | $33,000 |
| Family of 5 | $38,680 |
| Family of 6 | $44,360 |
| Family of 7 | $50,040 |
| Family of 8 | $55,720 |
| Family of 9+ | Add $5,680 for each extra person |
The 2026 FPL chart for Alaska is as follows:
| Household Size | Annual income Limit |
| 1 | $19,950 |
| 2 | $27,050 |
| 3 | $34,150 |
| 4 | $41,250 |
| 5 | $48,350 |
| 6 | $55,450 |
| 7 | $62,550 |
| 8 | $69,650 |
| For families/households with more than 8 persons, add $7,100 for each additional person. | |
The 2026 FPL chart for Hawaii is as follows:
| Household Size | Annual Income Limit |
| 1 | $18,360 |
| 2 | $24,890 |
| 3 | $31,420 |
| 4 | $37,950 |
| 5 | $44,480 |
| 6 | $51,010 |
| 7 | $57,540 |
| 8 | $64,070 |
| For families/households with more than 8 persons, add $6,530 for each additional person. | |
Income limits generally are based on Modified Adjusted Gross Income (MAGI). MAGI includes adjusted gross income, plus untaxed foreign income, non-taxable Social Security benefits and tax-exempt interest. It does not include Supplemental Security Income (SSI).
Aged, blind, and disabled individuals, as well as SSI recipients, are exempt from MAGI-based income requirements. Instead, they rely on SSI income calculations.
In addition, states have citizenship requirements. To be eligible for Medicaid, applicants should be a U.S. citizen or legal non-citizen, and be able to supply a Social Security Number (SSN) or an application for an SSN.
Asset limits may be required for MAGI-exempt Medicaid applicants. These limits involve measuring your liquid funds, such as bank accounts, CDs and investments. Your primary residence and one car are exempt from asset tests.
Note on Native American and Alaskan Native Eligibility for Medicaid:
u003c!u002du002d wp:paragraph u002du002du003ernrnNative American tribes and individuals who meet the requirements are eligible through Medicaid and all other programs funded through the Centers for Medicare and Medicaid Services. States may develop outreach programs to more effectively enroll Native Americans into Medicaid programs.rnrnu003c!u002du002d /wp:paragraph u002du002du003e u003c!u002du002d wp:paragraph u002du002du003ernrnNative Americans eligible for Medicaid u003cemu003edo notu003c/emu003e have to pay premiums, enrollment fees or out-of-pocket costs. Additionally, American Indian and Alaskan Native trust income is not counted when determining eligibility.rnrnu003c!u002du002d /wp:paragraph u002du002du003e
Note on Eligibility Group Abbreviations:
u003c!u002du002d wp:paragraph u002du002du003ernrnu003cstrongu003eQMBu003c/strongu003e refers to low-income Medicare beneficiaries.rnrnu003c!u002du002d /wp:paragraph u002du002du003e u003c!u002du002d wp:paragraph u002du002du003ernrnu003cstrongu003eSLMBu003c/strongu003e refers to Specified Low-Income Medicare Beneficiaries and refers to individuals with Medicare Part A and limited incomes.rnrnu003c!u002du002d /wp:paragraph u002du002du003e u003c!u002du002d wp:paragraph u002du002du003ernrnu003cstrongu003eWorking Disabledu003c/strongu003e individuals are disabled individuals who work to “buy in” to the Medicaid program when their income is higher than the standard income requirements.rnrnu003c!u002du002d /wp:paragraph u002du002du003e
Alabama
To qualify for Alabama Medicaid, the following must be true:
- All Medicaid beneficiaries must be Alabama residents.
- All Medicaid beneficiaries must be U.S. citizens or qualified U.S. residents.
- All Medicaid beneficiaries must meet the income eligibility requirements: https://medicaid.alabama.gov/documents/3.0_Apply/3.2_Qualifying_Medicaid/3.2_Medicaid_Income_Limits_2026_3-11-26.pdf
Eligibility for Children
- Children must be 18 years of age or younger.
Eligibility for Parents and Caretakers
- Applicants must have a close relative under the age of 19 living with them.
- Applicants must assign all medical insurance and support benefits to the state.
- Applicants must report all household changes immediately.
Eligibility for Pregnant Women
- Pregnant women under 19 years of age may receive full coverage if their parents’ income is counted and meets the income eligibility requirements.
Check to see if you meet Alabama’s income requirements for Medicaid here: https://www.benefits.gov/benefit/1618
Alaska
The Alaska Medicaid Eligibility requirements are as follows:
- Medicaid beneficiaries must be Alaska residents.
- Medicaid beneficiaries must be U.S. citizens or qualifying U.S. residents.
Check to see if you meet Alaska’s Medicaid eligibility requirements here: https://aries.alaska.gov/screener/accessScreener?id=0.2760063399882704
American Samoa
American Samoa does not have an application process or an eligibility checklist. The territory operates through presumptive eligibility.
American Samoa receives funding based on a calculation of the percentage of the population with income levels below 200 percent of the FPL. Qualifying residents automatically receive Medicaid based on that calculation.
Arizona
The Arizona Medicaid Eligibility requirements are as follows:
- Medicaid beneficiaries must be Arizona residents.
- Medicaid beneficiaries must be U.S. citizens or qualifying U.S. residents.
- Medicaid beneficiaries must have a Social Security Number.
Check to see if you meet the income requirements for Arizona Medicaid here: https://www.azahcccs.gov/Members/Downloads/EligibilityRequirements.pdf
Arkansas
To qualify for Arkansas Medicaid, all of the following must be true:
- You are a U.S. citizen, national, legal alien or permanent resident.
- You are a current Arkansas resident.
- You have a household income below 138 percent of the FPL, or below 200 percent of the FPL if you are a pregnant woman.
Most Arkansas Medicaid recipients meet at least one of the following qualifications:
- You are 65 years of age or older.
- You are 18 years of age or younger.
- You are blind or disabled.
- You are pregnant.
- You are a parent taking care of a child with an absent, unemployed or disabled parent.
- You are living in a nursing home.
- You are under 21 years of age and in the foster system.
- You medically require certain home and community-based services.
- You have breast cancer or cervical cancer.
- You are a parent or relative taking care of a child.
- You are between 19 and 64 years of age with a low income when participating in the ARHOME program
Check if you meet Arkansas’s Medicaid income requirements here: https://humanservices.arkansas.gov/wp-content/uploads/Quick-Reference-Medicaid-Chart-3.3.23.pdf
California
To qualify for California Medicaid, your household income must fall below 138 percent of the FPL.
You may also qualify for Medicaid in California if any of the following are true:
- You are 65 or older.
- You are blind or disabled.
- You are under 21.
- You are pregnant.
- You are in a nursing or intermediate care home.
- You have refugee status for a limited time.
- You are a parent or related caretaker of an age-eligible child.
- You have been screened for breast or cervical cancer.
- You are enrolled in CalFresh.
- You receive Supplemental Security Income or are enrolled in the State Supplemental Program.
- You are enrolled in CalWorks.
- You are enrolled in RefugeeAssistance.
- You are enrolled in the Foster Care or Adoption Assistance Program.
Check if you meet California’s Medicaid income eligibility requirements here: https://www.coveredca.com/see-if-you-qualify-for-financial-help/
Colorado
You may qualify for Medicaid in Colorado if you fall into any of the following groups:
- Children ages 0-18 with a household income under 260 percent of the FPL
- Pregnant women, over the age of 19, whose household income is under 260 percent of the FPL
- Parents and Caretaker Relatives (you must have a dependent child) whose household income does not exceed 133 percent of the FPL
- Adults without dependent children whose household income does not exceed 133 percent of the FPL
Check if you meet Colorado’s Medicaid eligibility requirements here: https://www.healthfirstcolorado.com/apply-now/do-you-qualify/
Commonwealth of Northern Mariana Islands
All individuals who receive SSI in the Northern Mariana Islands are eligible for Medicaid.
In addition, all individuals whose incomes and resources fall below 150 percent of the SSI income and resource standards are eligible as well.
Connecticut
You may qualify for Medicaid in Connecticut if you meet the following eligibility requirements (the income limits provided are total annual household income limits):
Check to see if you meet Connecticut Medicaid eligibility requirements here: https://portal.ct.gov/husky/how-to-qualify
Delaware
You may qualify for Medicaid in Delaware if you meet the following eligibility requirements:
- You are a Delaware resident.
- You are a citizen or legal non-citizen.
You must also meet these other eligibility requirements:
- Parents and caretakers must have a household income below 87 percent of the FPL.
- Children under 6 years of age must have a household income below 142 percent of the FPL.
- Children between 6 and 18 years of age must have a household income below 133 percent of the FPL.
- Adults with no children must have a household income below 133 percent of the FPL.
- Pregnant women must have a household income below 212 percent of the FPL.
Check to see if you meet Delaware’s Medicaid income eligibility requirements here: https://www.dhss.delaware.gov/dmma/fpl.html
District of Columbia
To qualify for Medicaid in the District of Columbia, you must be a resident of D.C. and a U.S. citizen or legal non-citizen. You must fall into one of the following groups:
- Children
- Youth
- Pregnant women
- Aged, blind or disabled individuals
- Low-income adults
Check the income requirements for Medicaid in the District of Columbia here: https://dhcf.dc.gov/node/892172
Florida
You must be a Florida resident and a U.S. citizen or legal non-citizen to qualify for Medicaid in Florida. In addition, you must fall into one of the following groups:
- Parents and caretakers for children
- Children 18 years of age or younger
- Pregnant women
- Former foster care recipients
- Non-citizens with medical emergencies
- Older and disabled individuals who do not receive Supplemental Security Income (SSI)
In general, your household income should fall below 133 percent of the FPL to qualify for Medicaid.
Check to see if you are eligible for Medicaid benefits in Florida here: https://www.myflfamilies.com/medicaid
Georgia
In Georgia, you may qualify for Medicaid if you are a Georgia resident and a U.S. citizen or legal non-citizen, and fall into any of the following categories:
- You think you are pregnant.
- You have been diagnosed with breast or cervical cancer.
- You are a child or teenager 18 years of age or younger.
- You are 65 years of age or older.
- You are blind.
- You have disabilities.
- You need nursing home care.
- You are part of a family with children under 19 and have very low or no income.
- You are a child who was adopted or in foster care.
Check to see if you meet Georgia Medicaid income eligibility requirements here: https://medicaid.georgia.gov/how-apply/basic-eligibility
If you are not eligible for traditional Medicaid, you could be eligible for Medicaid coverage through Georgia Pathways to Coverage, which aims to provide benefits to low-income Georgians ages 19-64. To qualify, you must have a household income up to 100% of the Federal Poverty Level (FPL). Learn more about Georgia to Pathways Coverage eligibility here: https://pathways.georgia.gov/eligibility
Guam
- Apply using the Application for Public Benefits.
- Download the form here: https://mybenefits.guam.gov/#/home
- When the form is complete, return it to DPHSS at:
DPHSS
123 Chalan Kareta
Mangilao, Guam 96913-6304
Hawaii
To qualify for Medicaid in Hawaii, you must meet the following requirements:
- Be a Hawaii resident.
- Be a U.S. citizen or a permanent legal non-citizen.
- Be a qualified non-citizen.
- Have a household income at or below 133 percent of the FPL, except for pregnant women and children up to age 6.
Check to see if you’re eligible for Medicaid in Hawaii by taking the Pre-Assessment here: https://medical.mybenefits.hawaii.gov/web/kolea/home-page
Idaho
In Idaho, you may be eligible for Medicaid if you meet the following requirements:
- You are a resident of Idaho.
- You are a U.S. citizen or legal permanent resident.
- You meet the income eligibility requirements.
Additionally, you must also meet one of the following requirements:
- You are under 19 years of age.
- You are a parent or caretaker of someone under 19 years of age.
- You are a pregnant woman.
- You are a woman diagnosed with breast cancer, cervical cancer or pre-cancer.
- You are 65 years of age or older.
- You are blind or disabled.
In general, adults can get Medicaid in Idaho if their income falls below 138 percent of the FPL.
Check to see if you meet the Idaho Medicaid income eligibility guidelines here: https://healthandwelfare.idaho.gov/medicaid-program-income-limits
Illinois
In Illinois, you must meet one of the following requirements in order to be eligible for Medicaid:
- You are blind or disabled.
- You are 65 years of age or older.
- You are a low-income adult between 19 and 65 years of age.
- You are a pregnant woman.
- You have children under the age of 19 years old.
- You are an adult between 19 and 26 years old who aged out of the foster system, regardless of income.
- You are a woman with breast or cervical cancer.
In addition, all applicants except children must be U.S. citizens or legal permanent residents.
The Illinois income eligibility requirements are:
- Adults and parents or caretakers must have a household income below 138 percent of the FPL.
- Seniors, disabled and blind individuals should have household incomes below 100 percent of the FPL.
- Children should have household incomes below 147 percent of the FPL for full Medicaid.
- Children should have household incomes below 318 percent of the FPL for partial Medicaid coverage.
- Pregnant women should have household incomes below 213 percent of the FPL.
- Women with breast or cervical cancer should have household incomes below 200 percent of the FPL.
- Workers with disabilities should have household incomes below 350 percent of the FPL.
- Qualified Medicare Beneficiaries should have household incomes below 135 percent of the FPL.
Check to see if you’re eligible for Illinois Medicaid benefits here: https://getcovered.illinois.gov/
Indiana
In Indiana, you must meet one of the following requirements in order to qualify for Medicaid:
- You are a low-income adult between 19 and 64 years of age.
- You are a low-income caretaker or parent with children below 19 years of age.
- You are a low-income pregnant woman.
- You are a foster child or former foster child up to 26 years of age.
- You are 65 years of age or older.
- You are blind or disabled.
In addition, you must be a U.S. citizen or permanent legal resident, as well as a current Indiana resident, to qualify for Medicaid in the state.
Check to see if you meet the Indiana Medicaid income eligibility guidelines here: https://www.in.gov/medicaid/members/apply-for-medicaid/eligibility-guide/
Iowa
In order to qualify for Medicaid in Iowa, you need to be an Iowa resident as well as a U.S. citizen. In addition, you must also fall into one of the following categories:
- A child under the age of 21
- A parent living with a child under the age of 18
- A woman who is pregnant
- A woman in need of treatment for breast or cervical cancer
- A person who is 65 years of age or older
- A person who is blind or disabled
- An adult between the ages of 19 and 64 and whose income is at or below 133 percent of the FPL
Your household income must generally fall below 133 percent of the FPL.
Check to see if you are eligible for Medicaid in Iowa here: https://hhsservices.iowa.gov/apspssp/ssp.portal
Kansas
In Kansas, you must be a U.S. citizen or permanent legal resident to receive Medicaid coverage. In addition, you must fall into one of the following categories:
- Children under 19 years of age
- Pregnant women
- Adult parents and caregivers
- Seniors, blind and disabled individuals
In general, your household income must fall below 133 percent of the FPL.
Check to see if you meet the Kansas Medicaid eligibility guidelines here: https://www.kancare.ks.gov/apply-now/eligibility
Kentucky
To qualify for Medicaid in Kentucky, you must be a Kentucky resident as well as a U.S. citizen or permanent legal resident. In addition, you must be part of a low-income household and belong to one of the following categories:
- Blind or disabled individuals
- Children under 19 years of age
- Adults or caretakers with children under 19 years of age
- Individuals under 26 years of age in the foster care program
- Pregnant women
In general, your household income must fall below 133 percent of the FPL.
Check to see if you meet the income eligibility guidelines for Medicaid in Kentucky here: https://kynect.ky.gov/benefits/s/medicaid-kchip-program?language=en_US
Louisiana
In order to receive Medicaid in Louisiana, you must be a Louisiana resident and a U.S. citizen, permanent resident or legal alien. In addition, you must fall into one of the following categories:
- You receive Supplemental Security Income from the Social Security Administration.
- You get financial help from the Office of Family Support.
- You are disabled or blind.
- You are a parent of children under age 19.
- You are under 19 years of age.
- You are a pregnant woman.
- You have no insurance and need treatment for breast and/or cervical cancer.
- You receive Medicare coverage and are low-income.
- You are an adult between 19 to 64 years of age.
You must meet the income requirements in Louisiana to get coverage. Most applicants must earn less than 138 percent of the FPL to receive coverage. Children need a household income below 255 percent of the FPL to get coverage. Workers with disabilities can get coverage if they earn less than 100 percent of the FPL.
Check to see if you meet the Louisiana Medicaid income eligibility guidelines here: https://ldh.la.gov/page/medicaid-eligibility-income-limits
Maine
In order to receive Medicaid in Maine, you must be a low-income Maine resident and a U.S. national, citizen, permanent resident or legal alien.
Additionally, you must fall into one of the following categories:
- Low-income adults between 19 and 64 years of age
- Children under 21 years of age
- Parent or caretaker of a child under 18 years of age
- Pregnant woman
- Aged, blind or disabled adult
- Adult working with a disability
Check to see if you meet the Maine income eligibility guidelines here: https://www.maine.gov/dhhs/ofi/programs-services/health-care-assistance
Maryland
To qualify for Medicaid in Maryland, you must be a Maryland resident as well as a U.S. citizen or legal resident. In addition, you must belong to one of the following categories:
- Low-income adults
- Children under 19 years of age
- Former foster care youth under 26 years of age
- Parents and caretakers of children under 19 years of age
- Disabled and blind individuals
- Low-income seniors over 65 years of age
- Pregnant women
- Medically needy individuals
- Disabled working adults
- Refugees
Check to see if you qualify for Medicaid in Maryland here: https://www.marylandhealthconnection.gov/shop-and-compare/medicaid-basics-and-benefits/
Massachusetts
In Massachusetts, you may qualify for Medicaid if you are a Massachusetts resident as well as a U.S. citizen or legal permanent resident. In addition, you must fall into one of the following categories:
- Parents or caretakers of children under 19 years of age
- Children under 19 years of age
- Adults between 20 and 64 years of age
- Pregnant women
- Disabled and blind adults
- Women with breast or cervical cancer
- Seniors and individuals who need long-term care
Check to see if you meet the income eligibility guidelines for Medicaid in Massachusetts here: https://www.mass.gov/info-details/program-financial-guidelines-for-certain-masshealth-applicants-and-members#2024-masshealth-income-standards-and-federal-poverty-guidelines-
Michigan
To qualify for Medicaid in Michigan, you must be a U.S. citizen or legal non-resident as well as a resident of the state of Michigan. You must also have an income below 133 percent of the FPL, in general. You must also fall into one of the following groups:
- Disabled or blind individuals
- Seniors
- Low-income families
- Low-income adults
- Children of low-income families
- Pregnant women
Minnesota
In order to qualify for Medicaid in Minnesota, you must meet the following eligibility requirements:
- You must be a U.S. citizen.
- You must be a resident of Minnesota.
- You must meet the income and asset limits.
Check to see if you are eligible for Medicaid in Minnesota here: https://www.benefits.gov/benefit/1286
Mississippi
To be eligible for Medicaid in Mississippi, you must be a U.S. citizen or legal permanent resident, as well as a Mississippi resident. You must also belong to one of the following groups:
- Infants and children between 0-18 years of age
- Parents and caretakers of minors
- Pregnant women
- Disabled or blind individuals
- Seniors
Check to see if you meet the Mississippi income eligibility guidelines here: https://medicaid.ms.gov/medicaid-coverage/who-qualifies-for-coverage/income-limits-for-medicaid-and-chip-programs/
Missouri
You may be eligible for Medicaid in Missouri if you are a U.S. citizen or qualified resident, a Missouri resident and you belong to one of the following qualifying groups:
- Disabled and blind individuals
- Seniors
- Pregnant women
- Children
- Uninsured women
- Families
- Women with breast or cervical cancer
Check to see if you meet the Missouri income eligibility guidelines here: https://mydss.mo.gov/benefit-program-income-limits
Montana
You may be eligible for Medicaid in Montana if you are a state resident as well as a U.S. citizen or legal non-resident.
You must also belong to one of the following groups:
- Pregnant women
- Parents or caretakers
- Aged, blind and disabled individuals
You should also check to see if you meet the income requirements. Generally, individuals should have a household income below 138 percent of the FPL to qualify.
Check to see if you meet the Montana income eligibility guidelines here: https://dphhs.mt.gov/healthcare/apply
Nebraska
You may be eligible for Medicaid in Nebraska if you are a state resident as well as a U.S. citizen or legal non-resident.
You should also belong to one of the following groups:
- Aged, blind or disabled individuals
- Children
- Pregnant women
- Parents or caretakers
- Former foster care youth
Your resources should not exceed $4,000 for an individual, $6,000 for a couple and $25 for each additional family member. Children and pregnant women are not subject to this limitation.
Check to see if you meet the income eligibility guidelines for Medicaid in Nebraska here: https://dhhs.ne.gov/Documents/FPL%20Eligibility.pdf
Nevada
You may be eligible for Medicaid in Nevada if you are a state resident as well as a U.S. citizen or legal non-resident.
You should also belong to one of the following groups:
- Children
- Pregnant women
- Low-income families
- Aged, blind and disabled individuals
- Former foster care youth
You must also meet the income requirements. In general, your household income should fall below 138 percent of the FPL to qualify for Medicaid in Nevada. Children can receive Medicaid if their household incomes fall below 205 percent of the FPL; working disabled individuals need to earn less than 250 percent of the FPL.
Check to see if you meet the Nevada income eligibility guidelines here: https://www.dss.nv.gov/access-nv/eligibility-payments-info-manual/income-limit-charts/
New Hampshire
You may be eligible for Medicaid in New Hampshire if you are a state resident as well as a U.S. citizen or legal non-resident. You should not be getting medical assistance from other states.
You must also belong to one of the following groups:
- Children
- Pregnant women
- Low-income families
- Low-income adults
- Aged, blind and disabled individuals
- Former foster care youth
Check to see if you meet the New Hampshire income eligibility guidelines here: https://www.dhhs.nh.gov/sites/g/files/ehbemt476/files/documents2/bfa-progam-fact-sheet.pdf
New Jersey
You may be eligible for Medicaid in New Jersey if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Families with dependent children
- Aged, blind or disabled individuals
- Children
- Pregnant women
- Disabled individuals
Check to see if you meet the New Jersey income eligibility guidelines here: https://njfamilycare.dhs.state.nj.us/who_eligbl.aspx
New Mexico
You may be eligible for Medicaid in New Mexico if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Families with dependent children
- Aged, blind and disabled individuals
- Children
- Pregnant women
- Disabled individuals
Check to see if you meet the income eligibility guidelines for Medicaid in New Mexico here: https://www.hca.nm.gov/wp-content/uploads/ISD-017-FPG-Cards-FY-2026-10.01.25-to-09.30.2026-final-1.pdf
New York
You may be eligible for Medicaid in New York if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Families with dependent children
- Aged, blind and disabled individuals
- Children
- Pregnant women
- Disabled individuals.
In general, low-income adults must earn less than 138 percent of the FPL.
Check to see if you meet the New York income eligibility guidelines here: https://www.nyc.gov/assets/ochia/downloads/pdf/all_populations_medicaid.pdf
North Carolina
You may be eligible for Medicaid in North Carolina if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Families with dependent children
- Aged, blind and disabled individuals
- Children
- Pregnant women
- Disabled individuals
Check to see if you meet the North Carolina income eligibility guidelines here: https://medicaid.ncdhhs.gov/eligibility
North Dakota
You may be eligible for Medicaid in North Dakota if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Low-income adults
- Children in foster care or subsidized adoption
- Former foster care children up to age 26, under certain circumstances
- Children with disabilities (birth to 19)
- Pregnant women
- Individuals with breast or cervical cancer
- Workers with disabilities
- Other blind and disabled individuals
- Low-income Medicare beneficiaries
Check to see if you meet the North Dakota income eligibility guidelines here: https://www.hhs.nd.gov/healthcare/medicaid/eligibility
Ohio
You may be eligible for Medicaid in Ohio if you are a state resident as well as a U.S. citizen or legal non-resident. You must also belong to one of the following groups:
- Individuals with low incomes
- Pregnant women, infants and children
- Older adults
- Parents and caretakers
- Individuals with disabilities
Check to see if you meet the Ohio income eligibility guidelines here: https://odh.ohio.gov/wps/wcm/connect/gov/2e3738aa-905a-4325-8839-e1172ca16fa9/2022+Ohio+Medicaid+Guidelines+%28web%29+02.01.22.pdf?MOD=AJPERES&CONVERT_TO=url&CACHEID=ROOTWORKSPACE.Z18_M1HGGIK0N0JO00QO9DDDDM3000-2e3738aa-905a-4325-8839-e1172ca16fa9-nX5WzUj#:~:text=Family%20Size%20Monthly%20Income*%201,not%20have%20private%20health%20insurance.
Oklahoma
In order to qualify for Medicaid in Oklahoma, you should be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you should belong to one of the following groups:
- Adults with children under 19
- Children under 19 and pregnant women
- Individuals 65 and older
- Individuals who are blind or who have disabilities
- Women under 65 in need of breast or cervical cancer treatment
- Men and women 19 and older with family planning needs
Check to see if you meet the Oklahoma income eligibility guidelines here: https://oklahoma.gov/ohca/individuals/mysoonercare/apply-for-soonercare-online/eligibility/income-guidelines.html
Oregon
In order to qualify for Medicaid in Oregon, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to an eligible group and meet the following income requirements:
- Children – 300 percent of FPL
- Low-income adults – 138 percent of FPL
- Pregnant women – 190 percent of FPL
Check to see if you meet the Oregon income eligibility guidelines here: https://www.oregon.gov/oha/HSD/OHP/Tools/HPE-Eligibility-Guide.pdf
Pennsylvania
In order to qualify for Medicaid in Pennsylvania, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Adults age 19-64
- Aged, blind and disabled individuals
- Families with children under age 21
You must also meet the income and resource requirements. In general, your income should fall below 133 percent of the FPL.
Check to see if you meet the income eligibility guidelines for Medicaid in Pennsylvania here: https://www.dhs.pa.gov/Services/Assistance/Pages/MA-General-Eligibility.aspx
Puerto Rico
All Puerto Rico residents below local Puerto Rico poverty level guidelines qualify for Medicaid. These are the income requirements:
| Household Size | Monthly Income Limit |
| 1 | $1,835.00 |
| 2 | $2,489.00 |
| 3 | $3,142.00 |
| 4 | $3,795.00 |
Rhode Island
In order to qualify for Medicaid in Rhode Island, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Adults with children 18 or younger
- Pregnant women
- Adults 65 years of age or older
- Adults with Special Needs
You must also meet the income requirements:
| Group | Income Limit |
|---|---|
| Parents and caretakers | 133 percent of FPL |
| Pregnant women | 253 percent of FPL |
| Children | 261 percent of FPL |
| Adults | 133 percent of FPL |
Check to see if you meet the income eligibility guidelines for Medicaid in Rhode Island here: https://eohhs.ri.gov/consumer/health-care
South Carolina
In order to qualify for Medicaid in South Carolina, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Children
- Pregnant women
- Parents and caretakers
- Women with breast or cervical cancer
- Disabled children
- Seniors, blind and disabled adults
- Former foster care adults
Check to see if you meet the income eligibility guidelines for Medicaid in South Carolina here: https://www.scdhhs.gov/members/program-eligibility-and-income-limits
South Dakota
In order to qualify for Medicaid in South Dakota, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Low-income families
- Children
- Pregnant women
- Disabled children
- Women with breast or cervical cancer
- Workers with disabilities
- Disabled adults
- Individuals in adult foster care facilities
- Individuals in assisted living facilities
- Elderly individuals
- Refugees
- Former foster care youth
Tennessee
In order to qualify for Medicaid in Tennessee, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Children under 19
- Pregnant women
- Parents and caretakers of children
- Women with breast or cervical cancer
- People who get SSI
- Institutionalized individuals
- Medically needy children up to age 21
Check to see if you meet the Tennessee income eligibility guidelines here: https://www.tn.gov/content/dam/tn/tenncare/documents/eligibilityrefguide.pdf
Texas
In order to qualify for Medicaid in Texas, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Low-income families
- Pregnant women
- Parents and caretakers
- Children
- Aged, disabled and blind individuals
- Former foster care recipients
You must also meet the income eligibility requirements where applicable:
| Group | Income Limit | Asset Limit |
|---|---|---|
| Children | 133 percent of FPL | None |
| Transitioning foster care youth, 18-20 | 413 percent of FPL | None |
| Pregnant women | 198 percent of FPL | None |
| Working with disabilities | 230 percent of FPL | $2,000 |
| Children with disabilities | 147 percent of FPL | None |
Check to see if you meet the Texas income eligibility guidelines here: https://www.hhs.texas.gov/services/health/medicaid-chip/medicaid-chip-programs-services/programs-children-families/medicaid-parents-caretakers
U.S. Virgin Islands
The U.S. Virgin Islands use local poverty levels to determine eligibility.
Individuals are eligible for Medicaid in the U.S. Virgin Islands if they fall below 133 percent of the USVI poverty level, which is equivalent to 102 percent of the FPL.
Disabled, blind and aged individuals can qualify with incomes up to 177 percent of the USVI poverty level, equivalent to 165 percent of the FPL.
U.S. Virgin Islands
- Apply using the Medicaid Application. Download the form here: https://www.dhs.gov.vi/financial_programs/documents/RevisedMedicaidApplication002.pdf
For questions about the application process, contact the Call Center at (340) 715-6929 or vimmis@dhs.vi.gov.
Utah
In order to qualify for Medicaid in Utah, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Low-income families
- Pregnant women
- Parents and caretakers
- Children
- Aged, disabled and blind individuals
- Women with breast or cervical cancer
You must have a household income below 133 percent of the FPL in general.
Check to see if you meet the Utah Income eligibility guidelines here: https://medicaid.utah.gov/ufaq/what-are-the-income-guidelines/
Vermont
In order to qualify for Medicaid in Vermont, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Low-income adults
- Pregnant women
- Parents and caretakers
- Children
- Aged, disabled and blind individuals
You must also meet the income requirements:
| Group | Income Limit |
|---|---|
| Children | 312 percent of FPL |
| Pregnant women | 208 percent of FPL |
| Adult | 133 percent of FPL |
| Working while disabled | 250 percent of FPL |
| Aged, disabled | 400 percent of FPL |
Check to see if you meet the Vermont Income eligibility guidelines here: https://info.healthconnect.vermont.gov/compare-plans/eligibility-tables/2026-eligibility-tables
Virginia
In order to qualify for Medicaid in Virginia, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Pregnant women
- Parents and caretakers of children 18 years of age or younger
- Children 18 years of age or younger
- Aged, disabled and blind individuals
You must meet the income requirements:
| Group | Income Limit |
|---|---|
| Children | 148 percent of FPL |
| Pregnant women | 148 percent of FPL |
| Adults | 138 percent of FPL |
| Aged, blind and disabled individuals | 80 percent of FPL |
| Working disabled | 80 percent of FPL |
Check to see if you meet the Vermont Income eligibility guidelines here: https://coverva.dmas.virginia.gov/learn/coverage-for-adults/adults-19-64-years-old/
Washington
In order to qualify for Medicaid in Washington, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. You must belong to one of the following groups:
- Low-income adults
- Very low-income parents or caretakers
- Pregnant women
- Children
- Aged, blind or disabled individuals
- Low-income Medicare recipients
- Former foster children
You must also meet the applicable income requirements:
| Group | Income Limit |
|---|---|
| Adults 19-64 years old | 138 percent of FPL |
| Parents or caretakers | 48 percent of FPL |
| Pregnant women | 198 percent of FPL |
| Children | 215 percent of FPL |
| Aged, Blind and Disabled | 74 percent of FPL |
Check to see if you meet the Washington Income eligibility guidelines here: https://www.hca.wa.gov/free-or-low-cost-health-care/i-need-medical-dental-or-vision-care/eligibility-overview
West Virginia
In order to qualify for Medicaid in West Virginia, you must be a resident of the state as well as a U.S. citizen or permanent legal resident. In addition, you must belong to one of the following groups:
- Children 18 years of age or younger
- SSI beneficiaries
- Very low-income families
- Pregnant women
- Seniors
- Blind and disabled individuals
- Women with breast or cervical cancer
In some cases, in order to get Medicaid in West Virginia, you must also meet the income requirements:
| Group | Income Limit |
|---|---|
| Children 0-1 | 163 percent of FPL |
| Children 1-6 | 146 percent of FPL |
| Children 6-19 | 138 percent of FPL |
| Pregnant women | 190 percent of FPL |
| Adults 19-65 | 138 percent of FPL |
Check to see if you meet the guidelines for Medicaid in West Virginia by screening for eligibility here: https://www.wvpath.wv.gov/
Wisconsin
In order to qualify for Medicaid in Wisconsin, you must be a Wisconsin resident and U.S. citizen or permanent legal resident. You must also belong to one of the following groups:
- Children 18 years of age or younger
- Seniors
- Low-Income adults
- Pregnant women
- People with disabilities
You must also meet the income and asset requirements for individual programs. Income limits can range from under 100 percent of FPL to 300 percent of FPL, depending on what program you are eligible for.
Check to see if you meet the Wisconsin Income eligibility guidelines here: https://www.dhs.wisconsin.gov/medicaid/fpl.htm
Wyoming
In order to qualify for Medicaid in Wyoming, you must be a Wyoming resident and a U.S. citizen or permanent legal resident. You must also belong to one of the following groups:
- Children
- Pregnant women
- Aged, blind or disabled individuals
- Parents or caretakers
- Women with breast or cervical cancer
In order to qualify for Medicaid in Wyoming, you must also meet the following eligibility requirements:
| Group | Income | Assets |
|---|---|---|
| Children 0-5 | 154 percent of FPL | None |
| Children 6-18 | 133 percent of FPL | None |
| Pregnant women | 154 percent of FPL | None |
| Aged, Blind or Disabled – Inpatient Care | 300 percent of FPL | 1 person – $2,0002 people – $3,000 |
| Qualified Medicare Beneficiary | 135 percent of FPL | 1 person – $7,8602 people – $11,800 |
| Specified Low-Income Medicare Beneficiary | 135 percent of FPL | 1 person – $7,8602 people – $11,800 |
| Parent or caretaker | 50 percent of FPL | None |
| Women with breast or cervical cancer | 250 percent of FPL | None |
| Working with disabilities | 300 percent of FPL | None |
Check to see if you meet the Wisconsin Income eligibility guidelines here: https://health.wyo.gov/healthcarefin/medicaid/programs-and-eligibility/medicaid-income-requirements/
How to Apply for Medicaid

In order to receive Medicaid benefits, you must submit an application with your state’s Medicaid office. Learn more about applying for Medicaid in the sections below.
When can you apply for Medicaid?
Unlike programs like Medicare or the Health Insurance Marketplace, you can apply for Medicaid benefits any time of year.
Documents Needed to Complete a Medicaid Application
To apply for Medicaid, you may need any of the following documents:
- The Social Security Number (SSN) or document number of all members of your household
- All employer and income documentation for all members of your household (including W-2s, 1099s and other wage and tax statements)
- Bank statements
Your state’s Medicaid application form will explain the exact documentation required to apply. Learn more in the section “How To Apply For Medicaid By State and Territory” of this guide.
Information Needed to Complete a Medicaid Application
To submit an application for Medicaid, you must complete an application form and may need to provide the following information for yourself and all other members of your household:
- Your name
- Your contact information
- Your address
- Your Social Security Number (SSN)
- The health insurance coverage you seek
- Your residency status
- Your citizenship status
- Your employment status
- Your household income
- Your household finances
- Your household property
- Your health insurance status
- Your tribal status
- Your veteran status
- Your current medical needs
- Your current expenses
- Your current benefits
Your state’s Medicaid application form will explain the exact information required in your state. Learn more in the section “How To Apply For Medicaid By State and Territory” on of this guide.
Medicaid Application Process
Depending on where you live, you may be able to apply for Medicaid in the following ways:
- Online
- When applying online, you can either apply directly with the federal government’s Health Insurance Marketplace (https://www.healthcare.gov/medicaid-chip/) or your state’s Medicaid website.
- In person
- By phone
- By mail
- By fax
- By email
Continue reading the section below to find the application methods available in each state. If you are a member of a federally recognized tribe, refer to the state wherein your tribe is located to learn how to apply.
How to Apply for Medicaid by State and Territory
To receive Medicaid benefits, you must submit a complete application through the Health Insurance Marketplace (https://www.healthcare.gov/medicaid-chip/) or with your state Medicaid agency. Learn how to apply for Medicaid by finding your state or territory in the list below.
Alabama
Apply online through Insure Alabama: https://insurealabama.adph.state.al.us
Apply by mail using the Application for Health Coverage & Help Paying Costs. Download and print the form here: https://medicaid.alabama.gov/content/9.0_Resources/9.4_Forms_Library/9.4.1_Applicant_Forms.aspx
If you cannot download the form, you can pick up a paper application at your local health department. Find a list of locations here: https://medicaid.alabama.gov/content/10.0_Contact/10.1_Medicaid_Contacts/10.1.1_Medicaid_Locations.aspx
When completed, mail the application to:
ALL Kids Program
P.O. Box 304839
Montgomery, AL 36130-4839
Alaska
Apply online through the Alaska Self-Service portal: https://aries.alaska.gov/screener/?logIn=N
Apply using the Application for Services. Download and print the form here: http://dpaweb.hss.state.ak.us/e-forms/pdf/GEN-50C.pdf
If you cannot download the form, you can request a paper application at your local Public Assistance Office. Find a list of offices here: https://dhss.alaska.gov/dpa/Pages/contacts.aspx
When the application is complete, mail or drop it off at your local Public Assistance Office.
Apply by phone by calling (800) 478-7778.
American Samoa
Contact the American Samoa Medicaid State Agency to learn how to apply:
- By phone: 1 (684) 699-4777
- By email: omr@medicaid.as.gov
- By mail:
ASTCA Executive Building #306
P.O. Box 6101
Pago Pago, AS 96799 - By fax: 1 (684) 699-4780
Arizona
Apply online through the Health-e-Plus Arizona portal: https://www.healthearizonaplus.gov/Login/Default
Apply by mail using a paper application. If you are over age 65, blind or disabled, use the Application for AHCCCS Medical Assistance and Medicare Savings Programs in English (https://www.azahcccs.gov/Members/Downloads/DE103.pdf) or Spanish (https://www.azahcccs.gov/Members/Downloads/DE103sp.pdf) and mail the completed form to:
AHCCCS Medical Assistance Specialty Programs
801 East Jefferson Street
Phoenix, AZ 85034
All other applicants can use the Application for Benefits in English (https://des.az.gov/sites/default/files/dl/FAA-0001A.pdf) or Spanish (https://des.az.gov/sites/default/files/dl/FAA-0001A-S.pdf) and mail the completed form to:
Arizona Department of Economic Security Family Assistance Administration
P.O. Box 19009
Phoenix, AZ 85005
Apply in person at your local DES Family Assistance Administration office. Find a list of locations here: https://des.az.gov/find-your-local-office
Arkansas
Apply online through Access Arkansas: https://access.arkansas.gov
Apply in person at the Department of Human Services (DHS) office in your county of residence. Find a map of locations here: https://humanservices.arkansas.gov/contact-us/county-office-map/
Apply using a Household Health Coverage Application. Download and print the form here: https://humanservices.arkansas.gov/wp-content/uploads/DCO-0152Combined.pdf
When the application is complete, mail it to:
DHS Pine Bluff Scanning Center
P.O. Box 8848
Pine Bluff, AR 71611-8848
Fax the form to 1-870-534-3421Email the form to 351Jefferson@arkansas.gov.
Drop the form off at your local DHS office.
California
Apply online through Covered California: https://www.coveredca.com/apply/apply-online/
Apply by mail using the Application for Health Insurance. Download and print the form here: https://www.dhcs.ca.gov/services/medi-cal/eligibility/Documents/2014_CoveredCA_Applications/ENG-CASingleStreamApp.pdf
When the application is complete, mail it to:
Covered California
P.O. Box 989725
West Sacramento, CA 95798-9725
Apply in person at your local County Social Services Office. Find a list of locations here: https://www.dhcs.ca.gov/services/medi-cal/Pages/CountyOffices.aspx
Colorado
Apply online through Colorado PEAK: https://peak.my.site.com/peak/s/peak-landing-page?language=en_US
Apply by mail using the Health First Colorado paper application. Download and print the form here: https://hcpf.colorado.gov/forms#by-mail
When the application is complete, mail it to:
Connect for Health Colorado
P.O. Box 35681
Colorado Springs, CO 80935
You can also mail it or drop it off at any Department of Human Services (DHS) office. A list of locations can be found on pages 37-40 of the application, or on the DHS website here: https://www.colorado.gov/cdhs/contact-your-county
Apply by phone at 1 (800) 221-3943 or State Relay at 711.
Apply in person at your local county DHS office or at an application assistance site. Find a list of application assistance offices here: https://apps.colorado.gov/apps/maps/hcpf.map
Commonwealth of Northern Mariana Islands
- Apply using the Application for Medical Assistance for the Needy. You can pick one up at the Medicaid office or download it here: https://medicaid.cnmi.mp/images/CNMI-images/PDFdocs/2019-09-04-Medicaid_Application_Form.pdf
- When the form is complete, return it to:
Government Bldg. No. 1252
Capitol Hill Rd. Caller Box 10007
Saipan, MP 96950
- When the form is complete, return it to:
Connecticut
- Apply online through Access Health CT: https://www.accesshealthct.com/AHCT/cthix/#/home
- Apply by phone at 1 (855) 805-4325.
- Apply in person at your local Department of Social Services (DSS) office. Find a list of locations here: https://portal.ct.gov/dss/About-the-Department-of-Social-Services/Contact
- Apply using paper application form AH3, available by calling Access Health CT at 1 (855) 805-4325. You can drop the form off or mail it to any DSS office.
Delaware
- Apply online through the ASSIST portal: https://signup.assistselfservice.dhss.delaware.gov/?destination=0
- Apply by mail using a paper application, which will be mailed to your home address. Call 1 (800) 372-2022 or (302) 255-9500 to be directed to the Division of Social Services (DSS) office closest to where you live. Appropriate application forms will be mailed to you.
- Complete, sign and date the application form in ink and mail it to the address provided on the form.
District of Columbia
- Apply online through DC Health Link: https://www.dchealthlink.com
- Apply using the Standard Application for Health Coverage & Help Paying Costs for Families (https://www.dchealthlink.com/sites/default/files/v2/forms/DC_Health_Link_Standard_Application_for_Help_Paying_for_Health_Coverage_201509.pdf) or individuals (https://www.dchealthlink.com/sites/default/files/v2/forms/DC_Health_Link_Application_for_Help_Paying_for_Health_Coverage_Short_201509.pdf)
- When the form is complete, either:
- Mail it to:
DC Health Link
DHS Case Records Management Unit
P.O. Box 91560
Washington, DC 20090 - Fax it to: (202) 671-4400.
- Mail it to:
- When the form is complete, either:
- Apply by phone at 1 (855) 532-5465.
- Apply in person at any ESA service center. Find a list of locations here: https://dhcf.dc.gov/service/how-apply-medical-coverage
Florida
Apply online through the ACCESS Florida portal: https://www.myflfamilies.com/myaccess
- Apply using the Family-Related Medicaid Application. Download the form here (https://palmbeach.floridahealth.gov/programs-and-services/clinical-and-nutrition-services/registration-forms-clinic-services/_documents/medicaid-application-english.pdf), print it out, complete it and mail it to:
ACCESS Central Mail Center
P.O. Box 1770
Ocala, Florida 34478-1770
Georgia
- Apply online through the Georgia Gateway portal: https://gateway.ga.gov/access/accessController?id=427a056ba982d864d159d2eec
- Apply in person at any Division of Family and Children Services office. Find a list of locations here: https://dfcs.georgia.gov/locations
- Apply by phone at 1 (877) 423-4746.
- Apply using Form 94A. Download the form here (https://dfcs.georgia.gov/services/how-do-i-apply-medicaid), print it, complete it and mail it to:
Division of Family and Children Services
Customer Contact Center
P.O. Box 4190
Albany, GA 31706
Hawaii
- Apply online through the Med-QUEST portal: https://medical.mybenefits.hawaii.gov/web/kolea/home-page
- Apply by phone at 1 (800) 603-1201 (toll-free), 1 (800) 316-8005 (toll-free TTY) or 711.
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://mybenefits.hawaii.gov/wp-content/uploads/2013/08/EditableDHS1100_092013.pdf
- When the form is complete, mail or fax it to one of the Med-QUEST eligibility units provided on page 9 of the application. You can also find a map of locations here: https://medquest.hawaii.gov/en/contact-us.html
Idaho
- Apply online using the Idalink portal: https://idalink.idaho.gov
- Apply by phone at 1 (877) 456-1233.
- Apply in person at any field office. Find a list of locations here: https://healthandwelfare.idaho.gov/offices
- Apply using the Application for Health Coverage Assistance. Download the form here: https://healthandwelfare.idaho.gov/FoodCashAssistance/HealthCoverageAssistance/HealthCoverageApplications/tabid/2883/Default.aspx
When the form is complete, you can either:
-
- Mail it to:
Self-Reliance Programs – Statewide Application Team
PO Box 83720
Boise, ID 83720-0026 - Fax it to 1-866-434-8278
- Email it to: MyBenefits@dhw.idaho.gov
- Mail it to:
Illinois
Apply online through the Application for Benefits Eligibility (ABE) portal: https://abe.illinois.gov/access/
Apply with a paper application. Download the form here: https://www.dhs.state.il.us/onenetlibrary/12/documents/Forms/IL444-2378B-IES.pdf
When the form is complete, mail, fax or drop it off at any Family Community Resource Center (FCRC). Find a list of locations here: https://www.dhs.state.il.us/page.aspx?module=12
Apply in person at any FCRC.
Indiana
- Apply online through the FSSA Benefits Portal: https://fssabenefits.in.gov/bp/#
- Apply in person at your local Division of Family Resources (DFR) office. Find a list of locations here: https://www.in.gov/fssa/dfr/2999.htm
- Apply by phone at 1 (800) 403-0864.
Iowa
- Apply online through the DHS Services Portal: https://hhsservices.iowa.gov/apspssp/ssp.portal
- Apply using the Application for Health Coverage and Help Paying Costs: https://dhs.iowa.gov/sites/default/files/470-5170.pdf?082420201334 (English)
https://dhs.iowa.gov/sites/default/files/470-5170S.pdf?082620201830 (Spanish)
When the form is complete, mail it to:
Imaging Center 4
PO Box 2027
Cedar Rapids, Iowa 52406
Kansas
- Apply online through the Medical Consumer Self-Service Portal: https://cssp.kees.ks.gov/apspssp/
- Apply using a paper application. https://www.kancare.ks.gov/apply-now
When the form is complete, fax it to the following numbers depending on your status:
If you are 65 years of age or older or have a disability, mail or fax your complete application to:
KanCare Clearinghouse
P.O. Box 3599
Topeka, KS 66601-9738
844-264-6285 (fax)
All others should mail or fax the complete application to:
KanCare Clearinghouse
P.O. Box 3599
Topeka, KS 66601-9738
800-498-1255 (fax)
Kentucky
- Apply online through the Benefind Portal: https://benefind.ky.gov
- Apply by phone at (855) 306-8959.
Louisiana
- Apply online through the Online Application portal: https://sspweb.lameds.ldh.la.gov/selfservice/
- Apply in person at a Medicaid Application Center. Find a list of locations here: https://ldh.la.gov/directory/category/159
Not all centers accept walk-ins. Call your local center before visiting. - Apply using the Application for Health Coverage. Download the form here: https://ldh.la.gov/assets/medicaid/MedicaidEligibilityForms/MedicaidApplicationPub.pdf
- When the form is complete, mail or fax it to:
Medicaid Application Office
P.O. Box 91278
Baton Rouge, LA 70821-9893
1 (877) 523-2987 (fax)
- When the form is complete, mail or fax it to:
Maine
- Apply online through My Maine Connection: https://www1.maine.gov/benefits/account/login.html
- Apply using the MaineCare application. Download the form here: https://www.maine.gov/dhhs/ofi/applications-forms
- When the form is complete, fax it to (207) 778-8429, email it to Farmington.DHHS@Maine.gov or mail it to:
Office for Family Independence
114 Corn Shop Lane
Farmington, ME 04938
- When the form is complete, fax it to (207) 778-8429, email it to Farmington.DHHS@Maine.gov or mail it to:
- Apply in person at a DHHS office. Find a list of locations here: https://www.maine.gov/dhhs/about/contact/offices
Maryland
- Apply online through Maryland Health Connection: https://www.marylandhealthconnection.gov
- Apply by phone at 1 (855) 642-8572 or 1 (855) 642-8573 (TTY).
- Apply in person at a Connector Entity (find locations here: https://www.marylandhealthconnection.gov/assets/Connector-Entity-Contact-Sheet.pdf), your local health department (find locations here: https://health.maryland.gov/Pages/departments.ASPX) or a Department of Social Services office (find locations here: https://mydhrbenefits.dhr.state.md.us/dashboardClient/#/dssMap)
- Apply through the Enroll MHC mobile app. Download it here: https://www.marylandhealthconnection.gov/enrollmhc/
Massachusetts
- Apply online through Massachusetts Health Connector: https://www.mahealthconnector.org
- Apply using the Massachusetts Application for Health and Dental Coverage and Help Paying Costs: https://www.mass.gov/doc/massachusetts-application-for-health-and-dental-coverage-and-help-paying-costs-0/download
- When the form is complete, mail or fax it to:
Health Insurance Processing Center
P.O. Box 4405
Taunton, MA 02780.
(857) 323-8300 (fax)
- When the form is complete, mail or fax it to:
- Apply by phone at (800) 841-2900 or (800) 497-4648 (TTY) Monday through Friday, 8 a.m. to 5 p.m.
- Apply in person at a MassHealth Enrollment Center (MEC) Monday through Friday, 8:45 a.m. to 5 p.m.. Find a list of locations here: https://www.mass.gov/service-details/masshealth-enrollment-centers-mecs
Michigan
- Apply online through MI Bridges: https://newmibridges.michigan.gov/s/isd-landing-page?language=en_US
- Apply by phone at 1 (855) 789-5610.
- Apply in person at your local Department of Human Services office. Find a map of locations here: https://www.michigan.gov/healthymiplan/0,5668,7-326-67920—,00.html
Minnesota
- Apply online through MNSure: https://auth.mnsure.org/RIDP/?account_type=Individual
- Apply using the MNSure paper application. Download the form here: https://edocs.dhs.state.mn.us/lfserver/Public/DHS-6696-ENG
- When the form is complete, mail it to one of the agency addresses found at the bottom of the application.
Mississippi
- Apply online through Access Mississippi: https://www.access.ms.gov
- Apply using the Mississippi Application for Health Benefits. Request a form be mailed to you by calling (800) 421-2408. Or, download the form here: https://medicaid.ms.gov/wp-content/uploads/2017/10/DOM_MAGIApp.pdf
- When the form is complete, mail it to the Mississippi Medicaid Regional Office that serves your county. Find a list of locations here: https://medicaid.ms.gov/about/office-locations/
- Or, fax the completed application to 601-576-4164
- Apply in person at a Mississippi Medicaid Regional Office.
Missouri
- Apply online through MyDSS: https://mydss.mo.gov/healthcare/apply
- Apply using the Application for MO Healthnet. Download the form here: https://dssmanuals.mo.gov/wp-content/uploads/2020/09/IM-1SSL-Fillable-Secured-6-24-21.pdf
- When the form is complete, mail or fax it to:
Greene County FSD
101 Park Central Square
Springfield, MO 65806
(417) 895-6080 (fax)
- When the form is complete, mail or fax it to:
Montana
- Apply online through the portal: https://apply.mt.gov/access/accessController?id=0.0457682247476211
- Apply by phone at 1 (800) 318-2596
- Apply in person at a Field Office of Public Assistance. Find a list of locations here: https://dphhs.mt.gov/hcsd/OfficeofPublicAssistance
Nebraska
- Apply online through the portal: https://apply.mt.gov/access/accessController?id=0.0457682247476211
- Apply by phone at 1 (800) 318-2596.
- Apply in person at a Field Office of Public Assistance. Find a list of locations here: https://dphhs.mt.gov/hcsd/OfficeofPublicAssistance
Nevada
- Apply online through ACCESS Nevada: https://accessnevada.dwss.nv.gov
- Apply using the Application for Health Insurance. Download the form here: https://dwss.nv.gov/uploadedFiles/dwssnvgov/content/Home/Features/Forms/2960-EG_Application%20for%20Health%20Insurance.pdf
- When the form is complete, mail it to your local welfare office. Find a list of Northern Offices here (https://dwss.nv.gov/Contact/Welfare_District_Offices-North/) and Southern offices here (https://dwss.nv.gov/Contact/Welfare_District_Offices-South/). You can also mail it to the DWSS state office at:
DWSS
P.O. Box 15400
Las Vegas, NV 89114
- When the form is complete, mail it to your local welfare office. Find a list of Northern Offices here (https://dwss.nv.gov/Contact/Welfare_District_Offices-North/) and Southern offices here (https://dwss.nv.gov/Contact/Welfare_District_Offices-South/). You can also mail it to the DWSS state office at:
New Hampshire
- Apply online through the NH EASY portal: https://nheasy.nh.gov/#/
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://nheasy.nh.gov/forms/E/800MA.pdf
- When the form is complete, mail or fax it to:
Central Medicaid Unit
129 Pleasant Street
Concord, NH 03301
(603) 271-8604 - Or, mail it to your local District Office. Find a list of offices here: https://www.dhhs.nh.gov/about-dhhs/locations-facilities
- When the form is complete, mail or fax it to:
- Apply by phone at 1-800-852-3345 ext. 9700.
New Jersey
- Apply online through NJ Family Care: https://www.njfamilycare.org
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://www.njfamilycare.org/docs/FC_APP-en.pdf
- When the form is complete, mail it to:
NJ FamilyCare
P.O. Box 8367
Trenton, NJ 08650-9802
- When the form is complete, mail it to:
New Mexico
- Apply online through the Yes NM portal: https://www.yes.state.nm.us/yesnm/home/index
- Apply using the Application for Assistance. Download the form here: https://www.hsd.state.nm.us/wp-content/uploads/HSD-100-English-revised-1.pdf
- When the form is complete, mail or fax it to:
Central ASPEN Scanning Area (CASA)
P.O. Box 830
Bernalillo, NM 87004
(855) 804-8960 (fax)
- When the form is complete, mail or fax it to:
- Apply by phone at (855) 637-6574.
New York
- Apply online through the NY State of Health Marketplace: https://nystateofhealth.ny.gov/individual
- Apply by phone at (800) 541-2831.
- Apply with a Certified Application Counselor or Navigator. Access the directory here: https://info.nystateofhealth.ny.gov/sites/default/files/August%202020%20Statewide%20Phone%20Enrollment%20Directory.pdf
- Apply in person at your local Department of Social Services (DSS). Find a list of locations here: https://www.health.ny.gov/health_care/medicaid/ldss.htm
North Carolina
- Apply online through ePASS: https://epass.nc.gov
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://policies.ncdhhs.gov/wp-content/uploads/dhb-5200-ia-9-2020.pdf
- When the form is complete, mail or drop it at your local Division of Social Services office (DSS). Find a list of locations here: https://www.ncdhhs.gov/divisions/social-services/local-dss-directory
- Apply in person at a DSS office.
- Apply by phone by calling your local DSS office.
North Dakota
- Apply online with the North Dakota DHS: https://dhsbenefits.dhs.nd.gov
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://apps.nd.gov/itd/recmgmt/rm/stFrm/eforms/Doc/sfn01909.pdf
- When the form is complete, mail it to:
ND DHS
600 East Boulevard Avenue Dept. 325
Bismarck, ND 58505
Or, mail it to your local Human Service Zone (also known as County Social Service Office). Find a list of locations here: https://www.hhs.nd.gov/human-service/zones
- When the form is complete, mail it to:
Ohio
- Apply online through the Ohio Benefits portal: https://benefits.ohio.gov/
- Apply in person at a Job and Family Services Office. Find a list of locations here: https://jfs.ohio.gov/County/County_Directory.pdf
- Apply by phone at (800) 324-8680.
Oklahoma
- Apply online through the Health Care Authority: https://www.apply.okhca.org/Site/UserAccountLogin.aspx
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://marketplace.cms.gov/applications-and-forms/marketplace-application-for-family.pdf
- When the form is complete, mail it to:
Health Insurance Marketplace
Dept. of Health and Human Services
465 Industrial Blvd.
London, KY 40750-0001
- When the form is complete, mail it to:
Oregon
- Apply online through the OregONE portal: https://one.oregon.gov
- Apply using the Application for Health Plan Benefits. Download the form here: https://www.oregon.gov/oha/HSD/OHP/Pages/apply.aspx#apps
- When the form is complete, mail or fax it to:
OHP Customer Service
P.O. Box 14015
Salem, OR 97309-5032
(503) 378-5628 (fax)
- When the form is complete, mail or fax it to:
- Apply in person at a Department of Human Services (ODHS) office. Find offices near you here: https://www.oregon.gov/odhs/Pages/office-finder.aspx
Pennsylvania
- Apply online through the COMPASS portal: https://www.compass.state.pa.us/compass.web/Public/CMPHome
- Apply by phone at 1 (866) 550-4355
- Apply using the Pennsylvania Application for Benefits. Download the form here: https://www.dhs.pa.gov/Services/Assistance/Documents/Benefits%20Applications/PA%200600-8-23-Final-uf.pdf
- When the form is complete, mail, fax or drop it off to your local County Assistance Office (CAO). Find a list of locations here: https://www.dhs.pa.gov/Services/Assistance/Pages/CAO-Contact.aspx
- Apply in person at your local CAO.
Puerto Rico
Apply online using the Streamline Application system: https://prod-ua.preeservices.com/
Rhode Island
- Apply online through HealthSource RI: https://healthsourceri.com/how-to-enroll/
- Apply in person at your local Department of human Services (DHS) office. Find a list of locations here: https://dhs.ri.gov/office-locator-tool
- Apply by phone at 1 (855) 840-4774.
South Carolina
- Apply online through South Carolina Healthy Connections: https://apply.scdhhs.gov/CitizenPortal/application.do
- Apply using the Application for Medicaid and Affordable Health Coverage. Download the form here: https://www.scdhhs.gov/sites/default/files/FM%203400.pdf
- When the form is complete, return it in one of the following ways:
- Email it to 8888201204@fax.scdhhs.gov
- Mail it to
SCDHHS-Central Mail
P.O. Box 100101
Columbia, SC 29202-3101 - Mail it to your local county office. Find a list of locations here: https://www.scdhhs.gov/site-page/where-go-help
- Apply in person at your local county office.
South Dakota
- Apply online through DSS South Dakota: https://dss.sd.gov/economicassistance/medical_eligibility.aspx
- Apply using the Application for Medicaid/CHIP, Health Coverage & Help Paying Costs. Download the form here: https://dss.sd.gov/formsandpubs/docs/MEDELGBLTY/FSSA.pdf
- When the form is complete, mail it to your local DSS office. Find a list of locations here: https://dss.sd.gov/findyourlocaloffice/
Tennessee
- Apply online through YourTexasBenefits: https://www.yourtexasbenefits.com/Learn/Home
- Apply using the paper application. Download the form or request a form by mail here: https://www.yourtexasbenefits.com/Learn/GetPaperForm
- When the form is complete, return it in one of the following ways:
- Mail it to:
HHSC
P.O. Box 149024
Austin, TX 78714-9968 - Fax it to 1 (877) 447-2839
- Drop it off at a benefits office. Search for your nearest office here https://hhs.texas.gov/about-hhs/find-us/where-can-i-find-services or call 2-1-1
- Apply in person at a Community Partner Program. Find a location here: https://www.texascommunitypartnerprogram.com
- Apply by phone Monday through Friday, 8:00 AM to 6:00 PM, at 1-877-541-7905 or 2-1-1
Texas
| Apply online through YourTexasBenefits: https://www.yourtexasbenefits.com/Learn/HomeApply using the paper application. Download the form or request a form by mail here: https://www.yourtexasbenefits.com/Learn/GetPaperForm When the form is complete, return it in one of the following ways:Mail it to:HHSCP.O. Box 149024Austin, TX 78714-9968Fax it to 1 (877) 447-2839Drop it off at a benefits office. Search for your nearest office here https://www.hhs.texas.gov/contact/hhs-locations or call 2-1-1Apply in person at a Community Partner Program. Find a location here: http://www.texascommunitypartnerprogram.com Apply by phone Monday through Friday, 8:00 AM to 6:00 PM, at 1-877-541-7905 or 2-1-1 |
Utah
- Apply online through myCase: https://jobs.utah.gov/mycase-app/ui/
- Apply using the Medical Application. Download the form here: https://medicaid.utah.gov/Documents/pdfs/61MED_English.pdf
- When the form is complete, return it in one of the following ways:
- Mail it to:
Department of Workforce Services
PO Box 143245
Salt Lake City, UT 84114-3245 - Fax it to (801) 526-9505
- Bring it to a Department of Workforce Services (DWS) office. Search for an office near you here: https://jobs.utah.gov/jsp/officesearch/#/map
- Mail it to:
- When the form is complete, return it in one of the following ways:
- Apply in person at a DWS office.
Vermont
- Apply online through Vermont Health Connect: https://vermonthealthconnect.gov
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://info.healthconnect.vermont.gov/sites/vhc/files/doc_library/205ALLMED%20Non-LTC%20%282023%29.pdf or call 1 (855) 899-9600 to have one mailed to you.
- When the form is complete, mail it to:
Vermont Health Connect
Application and Document Processing Center
280 State Drive
Waterbury, VT 05671-8100
- When the form is complete, mail it to:
- Apply by phone at 1 (855) 899-9600.
- Apply in person with an assister. Find one near you here: https://info.healthconnect.vermont.gov/find-local-help/find
Virginia
- Apply through the Virginia CommonHelp portal: https://www.commonhelp.virginia.gov
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://www.dmas.virginia.gov/media/rgaedgrg/magi-standard-application-final-03-01-2024.pdf
- When the form is complete, mail or drop it off at your local Department of Social Services (DSS) office. Find a list of locations here: https://www.dss.virginia.gov/localagency/
- Apply by phone at 1 (855) 242-8282 or 1 (888) 221-1590 (TTD) Monday through Friday, 8 a.m. to 7 p.m., and Saturday 9 a.m. to 12 p.m.
Washington
- Adults who are blind, disabled or 65 years of age or older can apply in the following ways:
- Online through Washington Connection: https://www.washingtonconnection.org/home/
- Using the Apple Health Application. Download the form here https://www.hca.wa.gov/assets/free-or-low-cost/18-005.pdf or call 1-877-501-2233 to request one by mail.
- When the form is complete, return it in one of the following ways:
- Mail it to:
DSHS
Community Services Division – Customer Service Center
P.O. Box 11699
Tacoma, WA 98411-6699 - Fax it to 1 (888) 338-7410
- Bring it to your local DSHS office. Find a list of locations here: https://www.dshs.wa.gov/office-locations
- In person at your local DSHS office
- Mail it to:
- When the form is complete, return it in one of the following ways:
- All other applicants can apply in the following ways:
- Online through Washington Healthplanfinder: https://www.wahealthplanfinder.org/_content/applynow.html
- Using the WAPlanfinder Mobile App. Download it here: https://www.wahbexchange.org/mobile/
- Using the Application for Health Care Coverage. Download the form here: https://www.hca.wa.gov/assets/free-or-low-cost/18-001P.pdf
- When the form is complete, mail it to:
Washington Healthplanfinder
P.O. Box 946
Olympia, Washington, 98507
You can also fax it to: 1 (855) 867-4467
- When the form is complete, mail it to:
- By phone at 1-855-923-4633
- In person with a Health Benefit Exchange Navigator. Find one near you here: https://www.wahealthplanfinder.org/HBEWeb/Annon_DisplayBrokerNavigatorSearch.action?brokerNavigator=NAV
West Virginia
- Apply online through WVPath: https://www.wvpath.wv.gov/
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://dhhr.wv.gov/bcf/Services/familyassistance/Documents/DFA_SLA_2%20%20Rev%2011_15.pdf
When the form is complete, mail, fax or bring it to your local DHHR office. Find a list of locations here: https://dhhr.wv.gov/bms/Pages/Field-Offices.aspx - Apply in person at your local DHHR office.
- Apply by phone at 1 (877) 716-1212.
Wisconsin
- Apply online through ACCESS Wisconsin: https://access.wi.gov/s/?language=en_US
- Apply using the Medicaid for the Elderly, Blind or Disabled packet (for adults who are blind, disabled or 65 years of age or older): https://www.dhs.wisconsin.gov/library/F-10101.htm or the BadgerCare Plus packet (for all other applicants): https://www.dhs.wisconsin.gov/forms/f1/f10182.pdf
- When the form is complete, mail it to:
CDPU
P.O. Box 5234
Janesville, WI 53547-5234
You can also fax it to: (855) 293-1822
*If you live in Milwaukee County, mail or fax it to:
MDPU
P.O. Box 05676
Milwaukee, WI 53205
(888) 409-1979 (fax)
- When the form is complete, mail it to:
- Apply by phone by calling your income maintenance or tribal agency. Find a list of contacts here: https://www.dhs.wisconsin.gov/forwardhealth/imagency/index.htm
- Apply in person at your income maintenance or tribal agency.
Wyoming
- Apply online through the Wyoming Eligibility System (WES): https://www.wesystem.wyo.gov/
- Apply using the Application for Health Coverage & Help Paying Costs. Download the form here: https://health.wyo.gov/healthcarefin/medicaid/index/
- When the form is complete, either:
- Mail it to:
WDH Customer Service Center
2232 Dell Range Blvd. #300
Cheyenne, WY 82009 - Email it to: wesapplications@wyo.gov
- Fax it to: 1 (855) 329-5205
- Apply by phone at 1 (855) 294-2127.
After Applying For Medicaid
In general, it takes up to 45 days for a state to review and approve your application for Medicaid. It can take up to 90 days if you require a disability determination as part of your application. However, the exact time frames may vary by state.
Incomplete applications or missing documents can take longer to process. Check your application and ensure it is complete before submitting it to avoid delays.
Note:
Although it can take up to 90 days for your benefits to be approved, they are retroactive. Once you are approved, your benefits will be approved from the day you applied. This means you will be reimbursed or covered for any eligible medical services you have received after submitting your application.
What happens after you are approved?
After you are approved for Medicaid, you will receive a letter informing you that you were approved. Soon afterwards, you will receive a Medicaid card that you can present as proof of coverage to obtain benefits.
If you require medical treatment after receiving your eligibility letter and before receiving your Medicaid card, you can present the letter as evidence that you qualify for benefits.
How long will your benefits last?
Medicaid benefits are not time-limited. You can continue to receive benefits as long as you remain eligible for them. However, you have to renew your benefits every year in order to continue receiving them. To renew your benefits, you should visit your state agency’s website and submit a renewal.
In the weeks before your renewal deadline, your state will contact you with information about how to renew your Medicaid benefits. Follow the instructions provided to complete the process.
If you experience any changes to your income, household size, disability status, expenses or other relative information, you must report it to your state’s Medicaid agency.
Medicaid Denials and Appeals

Your Medicaid application can be denied for many reasons. If your state or territory’s Medicaid agency believes you do not meet all the eligibility criteria, you will not receive Medicaid benefits. Although you can reapply for Medicaid in the future if your circumstances change, you can also appeal a denial if you believe you are entitled to Medicaid benefits.
Common Reasons for a Denial of Medicaid Benefits
You may be denied Medicaid benefits if you do not meet all of the eligibility criteria outlined by your state or territory’s Medicaid agency. To learn about eligibility criteria in your state or territory, refer to the “Medicaid Eligibility by State and Territory” section of this guide. Here are some of the most common reasons for being denied Medicaid:
- Your income exceeds your state or territory’s limit.
- You are not part of a covered population in your state or territory.
- You are not a legal U.S. resident.
- You have not met the five-year waiting period as a qualified non-citizen.
If you are denied Medicaid benefits, your state or territory will generally send you an eligibility determination notice detailing the reason that your application for Medicaid benefits was denied. This notice also describes the appropriate steps to take to file an appeal. This form may have a different name in some states and territories, such as a notice of denial or denial letter.
Requesting an Appeal
In many states and territories, you must request an appeal with the Medicaid agency. Some locations have a request form that you must complete, while others simply require you to send a letter expressing your request to an appeal.
The specific information needed in a written request can typically be found on the state or territory’s Medicaid agency website or webpage.
The information may vary slightly by location, but generally, you can expect to include the following information:
- Your full name
- If you are requesting on behalf of your family member, be sure to include both your and your family member’s name.
- If you will be represented by someone other than yourself during a requested hearing, including the representative’s name and phone number in the event the Medicaid agency wishes to contact him or her.
- Your home address
- Use the same home address you used on your Medicaid application.
- Your phone number
- The detailed reason for requesting an appeal
- Any supporting documents that may help your case and prove your eligibility for Medicaid
- A copy of the eligibility determination notice (if your state or territory sent you one)
How to File an Appeal in Each State and Territory
If you disagree with your denial and believe you qualify for Medicaid, you can appeal your state or territory’s decision. Most agencies require you to submit an appeal within a certain period of time of receiving an eligibility determination notice. The table below outlines these timeframes in each state and territory, as well as the appeal process and how to contact the governing body.
Note:
u003cspan style=u0022font-weight: 400;u0022u003eOne asterisk (*) indicates the information is not readily available. Contact your state or territory’s Medicaid agency for more information.u003c/spanu003eu003cspan style=u0022font-weight: 400;u0022u003e Find contact information in the “u003ca href=u0022#medicaid-contact-information-by-state-and-territoryu0022 target=u0022_blanku0022 rel=u0022noopeneru0022u003eMedicaid Contact Information By State and Territoryu003c/au003e” section of this guide.u003c/spanu003e
| State | Deadline to Appeal | How to Appeal | Appeals Contact Information |
|---|---|---|---|
| Alabama | Within 60 days of the date listed on the denial notice | File a written request for a fair hearing with the Alabama Medicaid Agency Appeals Office at: PO Box 5624 Montgomery, AL36103-5624 | Contact the hotline for assistance at 1 (800) 362-1504 / 1 (800) 253-0799 (TTY) or the Fair Hearings line at 1 (334) 242-5741. |
| Alaska | Within 30 days of the date listed on the denial notice | File a written request for appeal with the Office of Administrative Hearings by mailing your request to: P. O. Box 240808 Anchorage, AK 99524 Or, file a request via email at: fairhearings@conduent.com Or, file a request via fax at (907) 644-8126 | For additional information or assistance, contact the Recipient Helpline at 1 (800) 780-9972 or fairhearings@conduent.com |
| American Samoa | * | * | * |
| Arizona | Within 60 days of the date listed on the denial notice | Appeal verbally by phone or in writing to the agency listed on your notice of determination or decision (DES or AHCCCS). | Arizona Health Care Cost Containment System (AHCCCS)(602) 417-4000 Department of Economic Security Phone: (855) 432-7587 |
| Arkansas | Within 30 days of the date listed on the denial notice | Send a letter requesting a fair hearing to: DHS Office of Appeals and Hearings P.O. Box 1437, Slot N401 Little Rock, AR 72203-1437 Fax: (501) 404-4628 | DHS Office of Appeals and Hearings Phone: (501) 682-8622 |
| California | Within 60 days of receiving Notice of Action (NOA) | Complete the “Request for State Hearing” on the back of the Notice of Action (NOA) you receive and submit it to one of the following: By mail to the county welfare department at the address shown on the Notice of Action OR By mail to: The California Department of Social Services State Hearings Division P.O. Box 944243Mail Station 21-37 Sacramento, CA 94244-2430 OR By fax to the State Hearings Division by fax: (833) 281-0905 Alternatively, you may request an appeal online here: https://acms.dss.ca.gov/acms/login.request.do Or make a request by phone by calling 1 (800) 743-8525 (voice) / 1 (800) 952-8349 (TDD) | California Department of Social Services: Public Inquiry and Response Phone: 1 (800) 743-8525 |
| Colorado | Within 60 days of the date listed on the denial notice | Complete the Application for Hearing here: https://www.colorado.gov/oac/oac-form-links When complete, mail or fax it to: Office of Administrative Courts (OAC) Denver Office 1525 Sherman Street, 4th Floor Denver, CO 80203 Fax: (303) 866-5909 | Office of Administrative Courts (OAC) Phone: 1 (303) 866-2000 |
| Commonwealth of Northern Mariana Islands | * | * | * |
| Connecticut | Within 60 days of receiving Notice of Action (NOA) | The Notice of Action will include an Appeal Request form and explain how to submit an appeal. Appeal by phone at:1 (800) 859-9889 (you will still have to send an appeal notice in writing) Appeal in by mailing or faxing your appeal form to: State of Connecticut — Department of Social Services (DSS) Office of Legal Counsel Regulation and Administrative Hearings Husky A, C, D and Limited Benefit Appeals 55 Farmington Avenue, 11th floor Hartford, CT 06105 Fax: (860) 424-5729 | Member Engagement Services Phone: 1 (800) 859-9889 (Voice) / 711 (TTY for deaf or hard of hearing) |
| Delaware | Within 5 working days of receiving the notice | You will receive a notice that explains how to submit a request for a fair hearing. Request a fair hearing in writing to: DHSS Herman Holloway Campus, Lewis Building1901 N. DuPont Highway, New Castle, DE 19720 | DHSS Phone: (302) 255-9500 or 1 ( 800) 372-2022 |
| District of Columbia | Within 90 days of the postmark on your notice | Download, print and complete the Request for Hearing Form here: https://dhs.dc.gov/sites/default/files/dc/sites/dhs/release_content/attachments/FAIR%20HEARING%20FORM%20-%20English.pdf When complete, fax or email it to: Fax: (202) 724-2041Email: DC.OARA@DC.GOV OR Appeal by phone at: 1 (855) 532-5465 OR Appeal in person at: Administrative Hearings Resource Center441 4th Street NW, Suite 450-North, Washington, DC 20001 Or, appeal in person at any DHS Service Center. Find a list of locations here: https://dhs.dc.gov/service/find-service-center-near-you | Department of Human Services Economic Security Administration Phone: (202) 698-4147 |
| Florida | Within 90 days of receiving Notice of Action (NOA) | Request a fair hearing in one of three ways: Online here: https://ahca.myflorida.com/medicaid/florida-medicaid-complaints/medicaid-fair-hearings OR In writing and send by mail to: Appeal Hearings Section1317 Winewood Blvd., Bldg. 5Tallahassee, FL 32399-0700 OR By phone at 1 (850) 488-1429 | Office of Inspector GeneralAppeal Hearings Section Phone: 1 (850) 488-1429 Email: appeal.hearings@myflfamilies.com |
| Georgia | Within 45 days of the date listed on the notice | Appeal by phone at :1 (877) 423-4746 (Voice) / 1 (800) 255-0135 (TTY) OR Appeal in writing by mail, fax or email to: Right from Start Medical Assistance Group Attn: Eligibility Hearings Coordinator 426 West 12th Street Alma, GA 31510 Fax: (912) 632-0389 Email: RSM.mailfax@dch.ga.gov | Georgia Department of Community Health Phone: (404) 656-4507 |
| Guam | * | * | * |
| Hawaii | Within 90 days of receiving the notice | Request a review with the Med-QUEST Division by phone at (808) 692-8094. Request a review by mail or fax at: Health Care Services Branch P.O. Box 700190 Kapolei, HI 96709-0190 Fax: (808) 692-8087 | Med-QUEST Division Call the Med-QUEST unit nearest you. Find your local unit here: https://medquest.hawaii.gov/en/contact-us.html |
| Idaho | Within 28 days from the date the denial notice was mailed. | File an appeal or request a Fair Hearing Form by visiting your local Health and Welfare Office or by calling1 (877) 456-1233 Appeal in writing with your local Department of Health and Welfare office. Use the interactive map to find your nearest location here: https://healthandwelfare.idaho.gov/ContactUs/tabid/127/Default.aspx | Department of Health and Welfare Phone: 1 (877) 456-1233 |
| Illinois | Within 60 days of receiving the notice | Appeal online here: https://abe.illinois.gov/abe/access/appeals OR Call 1 (800) 435-0774 (voice) / 1 (877) 734-7429 (TTY) OR Write a letter or download, print and complete the appeal request form here: https://www.dhs.state.il.us/onenetlibrary/12/documents/forms/il444-0103.pdf When complete, mail, fax or email it to: Illinois Department of Human Services Bureau of Hearings 69 W. Washington, 4th Floor Chicago, IL 60602 Fax: (312) 793-3387 Email: DHS.BAH@Illinois.gov OR Mail or drop off your letter or completed appeals form at your local IDHS office. Find a list of locations here: https://www.dhs.state.il.us/page.aspx?module=12 | Illinois Department of Human Services (DHS) Phone: 1 (800) 843-6154 |
| Indiana | Within 60 days of the date listed on the notice | Follow the instructions on the denial notice you received from the Division of Family Resources (DFR). You may request an appeal in writing with the DFR by mail to: FSSA Document Center P.O. Box 1810 Marion, IN 46952 OR File an appeal request in person at your local DFR Office. Find a list of locations here: https://www.in.gov/fssa/dfr/2999.htm | Division of Family Resources Phone: 800-403-0864 |
| Iowa | Within 90 days of the date on your Notice of Decision | Submit an appeal letter explaining why you disagree with the decision by mail, fax or email at: Department of Human Services Appeals Section 1305 E Walnut Street, 5th Floor Des Moines, IA 50319 Fax: (515) 564-4044 Email: appeals@dhs.state.ia.us OR Appeal by phone at:(515) 281-3094 OR Appeal online using the appeal request form here: https://secureapp.dhs.state.ia.us/dhs_titan_public/appeals/appealrequest (English) / https://secureapp.dhs.state.ia.us/dhs_titan_public/appeals/appealrequest/1 (Spanish) | Department of Human Services Phone: (515) 281-3094 appeals@dhs.state.ia.us |
| Kansas | Within 60 days of the written notice | Mail a written request for a fair hearing to: 1020 South Kansas Avenue Topeka, KS 66612 | Office of Administrative Hearings Phone: (785) 296-2433 |
| Kentucky | Within 60 days of the written notice | Contact the Division of Administrative Hearings: Health Services Administrative Hearings branch to inquire about requesting a fair hearing | Health Services Administrative Hearings 105 Sea Hero Road Suite 2 Frankfort, KY 40601 CHFS.HSAHB@ky.gov Phone: (502) 564-6621 |
| Louisiana | Deadline listed on notice of denial | Complete an appeal request form online here: https://www.adminlaw.state.la.us/HH.htm OR Send a written request for appeal by mail or fax to: Division of Administrative LawHealth and Hospitals Section P. O. Box 4189 Baton Rouge, LA 70821-4189 Fax: (225) 219-9823 OR Request an appeal by phone at: (225) 342-5800 or (225) 342-0443 | Division of Administrative Law Phone: (225) 342-5800 |
| Maine | Within 30 days of the date of denial | Send a written request for appeal by email to: farmington.dhhs@maine.gov, or email the request to a regional office. Find a list of regional office contact information here: https://www.maine.gov/dhhs/about/contact/offices OR Mail a request for appeal to: Commissioner Dept. of Health and Human Services 11 State House Station Augusta, ME 04333 OR Request an appeal by phone at: 1 (855) 797-4357 OR Visit your local DHHS regional office and tell them you want to request an appeal. Find a list of regional office contact information here: https://www.maine.gov/dhhs/about/contact/offices | MaineCare Helpline1 Phone: (800) 965-7476 |
| Maryland | Within 90 days of receiving the notice | Download, print and complete the Request for Case Review here: https://www.marylandhealthconnection.gov/wp-content/uploads/2019/03/MHC.Appeals.Info_.Form_.pdf When complete, mail or email it to: Maryland Health Connection P.O. Box 857 Lanham, MD 20703-0857 or Office of Administrative Hearings 11101 Gilroy Road Hunt Valley, MD 21031 Email: MHBE.Appeals@maryland.gov OR Appeal by phone at: 1 (855) 642-8572 | Maryland Health Connection Phone: 1 (855) 642-8572 |
| Massachusetts | Within 30 days of receiving the notice | Download, print and complete the Fair Hearing Request Form here: https://www.mass.gov/doc/fair-hearing-request-form-2/download (English) / https://www.mass.gov/doc/como-pedir-una-audiencia-imparcial-4/download (Spanish) When complete, mail or fax it to: Office of Medicaid Board of Hearings 100 Hancock Street 6th Floor Quincy, MA 02171 Fax: (617) 887-8797 | Board of Hearings Phone: (617) 847-1200 |
| Michigan | Within 60 days of receiving the notice | Download, print and complete the Request for Fair Hearing form here: https://www.michigan.gov/documents/lara/Hearing_request_for_Medicaid_managed_care_Health_Plan_CMH_MI_CHoice_603943_7.pdf When complete, mail or fax it to: Michigan Department of Health and Human Services Michigan Administrative Hearing System P.O. Box 30763 Lansing, MI 48909 Fax: (517) 763-0146 | Michigan DHHS Administrative Hearing System Phone: 1 (800) 648-3397 |
| Minnesota | Within 30 days of receiving the notice | Complete an appeal request online using the fillable PDF here: https://edocs.dhs.state.mn.us/lfserver/Public/DHS-0033-ENG OR Download, print and complete the form here: https://edocs.dhs.state.mn.us/lfserver/Public/DHS-0033-ENG-pform When complete, mail or fax it to: Minnesota Department of Human Services Appeals Office P.O. Box 64941 St. Paul, MN 55164-0941 Fax: (651) 431-7523 | Department of Human Services: Appeals Division Phone: (651) 431-3600 |
| Mississippi | Within 30 days from the date of mailing on your notice | Request an appeal in writing by writing your own statement or using the General Inquiry Form here: https://medicaid.ms.gov/general-inquiry-form/ Mail, fax or deliver a written request to the regional office listed on your notice of denial | Office of Eligibility Phone: (800) 421-2408 |
| Missouri | Within 60 days of the date of denial | Contact the Division of Legal Services to inquire about requesting a fair hearing | Office of Appeals Phone: (800) 421-2408 Central Missouri Office Phone: (573) 751-0335 P.O. Box 1527 Jefferson City, MO 65102 DLS.JCIMHRG@dss.mo.gov Western Missouri Office Phone: (816) 325-5918 103 N Main, #202 Independence, MO 64050 DLS.KCIMHRG@dss.mo.gov Eastern Missouri Office Phone: (314) 877-20728 501 Lucas and Hunt, Suite 110 St. Louis, MO 63136 DLS.STLIMHRG@dss.mo.gov |
| Montana | Within 90 days of the mailing date of the notice | Submit a written request for a fair hearing to: Department of Public Health and Human Services Office of Fair Hearings PO Box 2029532 401 Colonial Drive, Third Floor Helena, MT 59620 Fax: (406) 444-3980 hhsofh@mt.gov | Office of Fair Hearings Phone: (406) 444-2470 |
| Nebraska | Within 90 days of receiving the notice | File written or verbal request for appeal with the Heritage Health Plan. Use the online contact form here: https://www.neheritagehealth.com/home/contact OR File an appeal by calling Nebraska Heritage Health | Nebraska Heritage Health Phone: 1 (888) 255-2605 |
| Nevada | Within 90 days of the date of eligibility determination on the eligibility correspondence you receive | Appeal online here: https://www.nevadahealthlink.com/appeals/ OR Download, print and complete the Appeals Request Form here: https://www.medicaid.nv.gov/downloads/provider/FA-90.pdf When complete, mail it to: Nevada Health Link Attn.: Appeals 2310 S. Carson Street, Suite 2 Carson City, NV 89701 OR Appeal by phone at: 1 (800) 547-2927 | Nevada HealthLink Call Center Phone: 1 (800) 547-2927 |
| New Hampshire | The Department must receive your appeal request within 30 days of the date written on the notice | Download, print and complete the Appeal Request Form here: https://www.dhhs.nh.gov/sites/g/files/ehbemt476/files/documents2/appeal-request.pdf When complete, mail it along with your denial notice/decision to: Administrative Appeals UnitMain Building 105 Pleasant Street Concord, NH 03301 | Administrative Appeals Unit Phone: 1 (800) 852-3345 ext. 4292 |
| New Jersey | Within 20 days of the date on your Eligibility Determination Notice | The appeals process varies based on the program for which you are denied. Learn about all appeals processes here: https://nj.gov/getcoverednj/findanswers/after/appealform.pdf | Medicaid Fair Hearing Unit Phone: (609) 588-2655 P.O. Box 712 Trenton, NJ 08625-0712 |
| New Mexico | Within 90 days of the date on your Eligibility Determination Notice | Request a fair hearing by phone at: 1 (800) 432-6217 or (505) 827-8164 OR Request a fair hearing by mail at: HSD Hearings Bureau P.O. Box 2348 Santa Fe, NM 87504 | New Mexico Medicaid Portal Phone: (800) 283-4465 |
| New York | Within 60 days of receiving the notice | Request a fair hearing using the online request system here: https://otda.ny.gov/hearings/request/ OR Download, print and complete the Fair Hearing Request Form here: https://otda.ny.gov/hearings/forms/request.pdf When complete, mail or fax it to: New York State Office of Temporary and Disability Assistance Office of Administrative Hearings P.O. Box 1930 Albany, NY 12201-1930 Fax: (518) 473-6735 OR Request a hearing by phone at:1 (800) 342-3334 OR If you live in New York City or Albany, you can request a fair hearing in person at the following office locations: Office of Temporary and Disability Assistance Administrative Hearings 14 Boerum Place, 1st Floor Brooklyn, NY 11201 Office of Temporary and Disability Assistance Administrative Hearings 40 North Pearl Street Albany, NY 12243 | Office of Administrative Hearings Phone: 1 (800) 342-3334 |
| North Carolina | Within 30 days of receiving the notice | Complete and return the Medicaid Services Recipient Hearing Request Form, which is included in the adverse decision notice. Mail or fax it to: 1711 New Hope Church Road Raleigh NC, 27609 Fax: (984) 236-1871 | Office of Administrative Hearings Phone: (984) 236-1850 |
| North Dakota | Within 30 days of the date on the notice of action | Download, print and complete the Request for Hearing form here: https://www.nd.gov/eforms/Doc/sfn00162.pdf When complete, mail, fax or email it to:Appeals Supervisor, Legal Advisory Unit Department of Human Services 600 E Boulevard Ave., Dept. 325 Bismarck, ND 58505-0250 Fax: (701) 328-2173 Email: dhslau@nd.gov | Department of Human Services Phone: (701) 328-2311 |
| Ohio | Department must receive your request within 90 days of the mailing date on notice of action | If you are denied services, you will receive a State Hearing Request form. Complete and return it to: Ohio Department of Job and Family Services Bureau of State Hearings P.O. Box 182825 Columbus, OH 43218-2825 OR Fax a request for a State Hearing to: (614) 728-9574 | Ohio Medicaid Consumer Hotline Phone: (800) 324-8680 |
| Oklahoma | Within 30 days of the date the OHCA sends written notice of action | Call (405) 522-7431 to request a form by mail When complete, mail it to: Oklahoma Health Care Authority 4345 N Lincoln Blvd. Oklahoma City, OK 73105 | Oklahoma Health Care Authority (OHCA) Phone: (405) 522-7300 |
| Oregon | Within 60 days of receiving the notice | Download, print and complete the Administrative Hearing Request form here: https://sharedsystems.dhsoha.state.or.us/DHSForms/Served/me0443.pdf When complete, mail or return to your local OHA or DHS office. A list of OHA offices can be found here: https://www.oregon.gov/oha/Pages/Contact-Us.aspx A list of DHS offices can be found here: https://www.oregon.gov/dhs/offices/pages/index.aspx | Oregon Health Authority Phone: (800) 375-2863 |
| Pennsylvania | Within 30 days of the mailing date on your letter | Download, print and complete the Fair Hearing Form here: https://services.dpw.state.pa.us/oimpolicymanuals/ma/PA-FS_162_F_7-14.pdf When complete, mail or bring it to your county’s assistance office (CAO). Find a list of locations here: https://www.dhs.pa.gov/Services/Assistance/Pages/CAO-Contact.aspx | Statewide Customer Service Center Phone: (877) 395-8930 |
| Puerto Rico | * | * | * |
| Rhode Island | Within 35 days of the date on the top of your letter | Download, print and complete the Appeal Form here: https://www.dhs.ri.gov/Programs/OHHS-121AppealsInstructionsandFormRev11-29-16.pdf When complete, mail it to: ATTN: Appeals State of Rhode Island P.O. Box 8709 Cranston, RI 02920-8787 OR Submit an appeal by phone at: 1 (855) 840-4774 OR Appeal in person at any DHS office. A list of locations can be found here: https://dhs.ri.gov/about-us/dhs-offices | Department of Human Services Phone: 1 (855) 697-4347 |
| South Carolina | Within 30 days of the mailing date on your letter | File an appeal online using the Eligibility Appeals form here: https://msp.scdhhs.gov/appeals/webform/eligibility-appeals OR File a written appeal by mail, fax or email to: SCDHHS Attn: Eligibility Appeals P.O. Box 100101 Columbia, SC 29202 Fax: (803) 255-8274 or (888) 835-2086 Email: eligappeals@scdhhs.gov | Division of Appeals and Hearings Phone: (803) 898-2600 or (800) 763-9087 |
| South Dakota | Within 30 days of the decision date from South Dakota Medicaid | Request a fair hearing by mailing a letter to: Department of Social Services Office of Administrative Hearings 700 Governors Drive Pierre, SD 57501 OR Submit a request by sending an email to: admhrngs@dss.state.sd.us | Department of Social Services Phone: 1 (800) 597-1603 |
| Tennessee | Within 60 days of the mailing date on your letter | Download, print and complete the appeal form here: https://www.tn.gov/content/dam/tn/tenncare/documents/RequestWilsonHearingForm.pdf When complete, mail or fax it to: TennCare Connect P.O. Box 305240 Nashville,TN 37230-5240 Fax: 1 (855) 315-0669 OR Appeal by phone at: 1 (855) 259-0701 | TennCare Connect Phone: 1 (855) 259-0701 |
| Texas | Within 90 days of receiving the notice | Appeal instructions are included in the notice of denial. If you have not received a notice, call 2-1-1 or contact the Appeals Division for assistance. | Appeals Division (512) 231-5701 |
| U.S. Virgin Islands | * | * | * |
| Utah | Within 90 days from the date the Medicaid Agency sent a denial notice | Download, print and complete the Hearing Request form here: https://jobs.utah.gov/appeals/490.pdf When complete, mail it via US Post Office to: Director’s Office / Administrative Hearings Division of Medicaid and Health Financing PO Box 143105 Salt Lake City, UT 84114-3105 Or, mail it via FedEx or UPS to:Director’s Office / Administrative Hearings Division of Medicaid and Health Financing 288 North 1460 West Salt Lake City, UT 84116-3231 You may also return it by fax (801-536-0143) or email (administrativehearings@utah.gov) | Division of Medicaid and Health Financing Phone: (801) 538-6576 |
| Vermont | Within 90 days of the mailing date on your letter | File a written appeal by mailing a request to: Vermont Health Connect 280 State Dr. Waterbury, VT 05671 Or Email a request to: AHS.DVHAHealthCareAppealsTeam@vermont.gov Or Appeal by phone at: 1 (855) 899-9600 Or If you have a Vermont Health Connect account, file an appeal online here: https://identity.id.vermont.gov/ After you log in, click on “My Requests.” | Vermont Health Connect Phone: (855) 899-9600 |
| Virginia | 30 days or the time limit on your written notice | Email a request for appeal to: appeals@dmas.virginia.gov OR Appeal by phone at: (804) 371‐8488 (Voice) / 1 (800) 828-1120 (TTY) | Department of Medical Assistance Services (DMAS) Phone: (804) 371‐8488 |
| Washington | * | If you are denied benefits, you will receive an appeal request form. Complete the form and fax it to: 1 (360) 586-9080 OR Call 1 (855) 923-4633 or 1 (800) 562-3022 | Office of Administrative Hearings Phone: 800-583-8271 |
| West Virginia | Within 90 days of the mailing date on your letter | Contact the Board of Review to inquire about Medicaid eligibility appeals | Board of Review State Capitol Complex Building 6, Room 817-B Charleston, WV 25305 Phone: (304) 558-0955 dhhroigbore@wv.gov |
| Wisconsin | Within 45 days from the date of the notice or within 45 days from the effective date of the decision announced in the notice, whichever is later | Send a written request for appeal to: Department of Administration Division of Hearings and Appeals P.O. Box 7875 Madison, WI 53707 OR Appeal by phone at: 1 (608) 266-3096 | Department of Health Services Phone: (800) 362-3002 |
| Wyoming | Within 30 days of being notified | To request an appeal, contact the contact the Customer Service Center | Medicaid Customer Service Center Phone: 1 (855) 294-2127 |
Medicaid Cost-Sharing
States have the ability to charge Medicaid recipients for health care services in order to offset the cost of providing medical services. These payments are known as:
- Premiums: Monthly fees you pay to your state Medicaid program for enrolling in and maintaining Medicaid health coverage. States can either charge premiums per person or per family.
- Copayments: Fees you pay to your health care provider in exchange for receiving health care services. These fees are sometimes called “copays” or “cost-sharing” payments.
Who is exempt from copayments?
According to federal Medicaid regulations, the following individuals do not need to make any copayments for services, regardless of where they live:
- American Indian and Alaska Natives who have previously received a service from the Indian Health Service (IHS), tribal health programs or under contract health services referral
- Children younger than age 18 (states may choose to extend this exclusion to 19, 20 or 21 years of age)
- Individuals living in an institution who contribute almost all of their income toward the cost of care
- Individuals receiving hospice care
- Women receiving Medicaid through the Breast and Cervical Cancer Treatment Program (exempt only from alternative out of pocket costs)
Which services are exempt from copayments?
In addition to the above groups, certain services are exempt from copayments by federal law. Exempted services include:
- Emergency services
- Family planning services
- Pregnancy-related services
- Preventive services for children
States may choose to exclude additional groups of people or services from copayments, but they are required to at least uphold these federal exclusions. For a list of additional copayment exclusions by state, continue reading below.
Who can be charged premiums under Medicaid?
Some states require some certain Medicaid beneficiaries to pay premiums or monthly contributions, otherwise known as enrollment or maintenance fees. They are:
- Arkansas
- California
- Indiana
- Iowa
- Michigan
- Montana
Only the following groups of people can be charged premiums under federal Medicaid regulations:
- Pregnant women and infants with household incomes at or above 150 percent of the FPL
- Disabled and working individuals with household incomes at or above 150 percent of the FPL
- Disabled working individuals who qualify under the Ticket to Work and Work Incentives Improvement Act of 1999
- Disabled children who qualify under the Family Opportunity Act
- Medically needy individuals
States have the ability to impose premiums on other groups of people whose household income exceeds 150 percent of the FPL.
Medicaid Copayments by State and Territory
Note:
This section does not include federally-exempt groups or federally exempt services.
Alabama
In addition to federal exclusions, the following individuals are exempt from copayments:
- Individuals in nursing homes
- Individual younger than 18 years of age
- Pregnant women
- Native American Indians with an active user letter from the Indian Health Services (IHS)
| Service | Copay |
| Non-preventative physician visit | Between $1.30 – $3.90 per visit |
| Prescriptions | Between $0.65 – $3.90 per drug |
| Inpatient hospital visits | $50 |
Alaska
In addition to federal exclusions, the following individuals are exempt from copayments:
- Participants who are eligible for both Medicare and Medicaid if Medicare is the primary payer for the service
- Chronic and Acute Medical Assistance (CAMA) recipients
- Children 17 years of age and younger
- Pregnant women
| Service | Copay |
| Non-preventative physician visit | $3 per visit |
| Visits to a health care provider or clinic | $3 per visit |
| Outpatient hospital services (except emergencies) | 5 percent of the allowed amount |
| Inpatient hospital visits | $50 per day, $200 maximum |
| Prescriptions | $.50 per prescription that costs $50 or less; $3.50 per prescription that costs more than $50 |
Arizona
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children 18 years of age and younger
- Individuals who are determined to be Seriously Mentally Ill (SMI) by the Department of Health Services
- Individuals enrolled in the Arizona Long Term Care System
- Individuals enrolled in the Children’s Rehabilitative Services program
- Anyone enrolled in Medicare
- Individuals in nursing homes
- Individuals receiving hospice care
- Women enrolled in the Breast and Cervical Cancer program
- Pregnant women
- Postpartum women
- Native American Indian members who are active or previous users of the Indian Health Service, tribal health programs or urban Indian health programs
- Individuals receiving Title IV-E Adoption Subsidy or Foster Care Assistance
- Individuals receiving Title IV-B Child Welfare Services
- Anyone receiving emergency services or hospitalization
| Service | Copay |
| Office visit | $3.40 – $4 |
| Outpatient therapy | $2.30 – $3 |
| Prescriptions | $2.30 |
| Non-emergency surgery | $3 |
| Non-emergency use of emergency room | $8 |
Arkansas
Cost-sharing begins at 21% of the federal poverty line. Copay annual limit is $27-$163, based on household FPL.
| Service | Copay |
| Non-preventative physician visit | $4.70 per visit |
| Prescriptions | $4.70 for generic drugs and preferred brand name drugs; $9.40 for non-preferred brand name drugs |
California
Most Medi-Cal enrollees do not pay any monthly premiums, copayments or out-of-pocket costs. However, some beneficiaries may need to pay a copayment of $1 each time they receive a prescription medication, dental service or medical service. They may need to pay $5 when they visit an emergency room (ER) for non-emergencies. Some families enrolled in Medi-Cal may need to pay monthly premiums of $13 per child up to a maximum of $39 per month.
Colorado
In addition to federal exclusions, children younger than 19 years of age and pregnant women are exempt from copayments.
| Service | Copay |
| Non-emergency visits to emergency room | $8 per visit |
Connecticut
Individuals enrolled in the following Medicaid plans do not pay any copayments or out-of-pocket costs for services:
- Husky A: Open to children, their families and pregnant women who meet income requirements
- Husky C: Open to adults older than 65 years of age as well as blind or disabled individuals between the ages of 18 and 65
- Husky D: Open to adults between the ages of 19 and 65 who do not qualify for Medicare, do not qualify for Husky A, do not have dependent children and are not pregnant
Children enrolled in Husky B (CHIP) may need to make copayments and pay premiums for services.
Delaware
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than age 21 years of age
- Pregnant women up to 1 year after end of pregnancy
- Chronic Renal Disease Program (CRDP) members
- Long-term care nursing facility group or the acute care hospital group
Copayments range between $0.50-$3.00.Prescription drug copays are based on the cost of the medication, with copay costs varying
District of Columbia
Washington DC residents enrolled in Medicaid do not pay any copayments for services unless they are in a fee-for-service (FFS) plan. FFS enrollees pay a $1 copay for prescriptions and a $2 copay for eyeglasses.
Florida
In addition to federal exclusions, the following individuals are exempt from copayments:
- Individuals enrolled in a Medicaid prepaid health plan or health maintenance organization
- Children younger than 21 years of age
- Pregnant women up to six weeks after end of pregnancy
- Individuals requiring emergency services for a condition which, if left untreated, places their health in jeopardy
| Service | Copay |
| Doctor visit | $2 per visit |
| Hospital outpatient visits | $3 per visit |
| Prescriptions | 2.5 percent of the Medicaid cost of the drug for a maximum of $7.50 per prescription |
| Non-emergency visit to the emergency room | Maximum $15 per visit |
Georgia
In addition to federal exclusions, children younger than 21 years of age and pregnant women are exempt from copayments:
| Service | Copay |
| Prescriptions | $.50 – $3 per prescription |
| Outpatient Visits (non-emergency) | $3 per visit |
| Inpatient Visits | $12.50 per visit |
| Ambulatory surgical center | $3 per visit |
| Federally qualified & rural health centers | $2 per visit |
| Non-emergency visit to emergency room | $3 per visit |
| Oral maxillofacial | $.50 – $3 per visit |
| Emergency room prescriptions | No copay |
Hawaii
Hawaii residents enrolled in Medicaid do not pay any monthly premiums, copayments or out-of-pocket costs for services.
Idaho
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 19 years of age with a family income of 133 percent FPL or lower
- Adults 19 years of age or older with a family income of 100 percent FPL or lower
- Members admitted to a hospital, nursing facility or intermediate care facility with intellectual disabilities
- Children in foster care receiving aid or assistance under Title IV, Part B of the Social Security Act
- Members receiving adoption or foster care assistance under Title IV, Part E of the Social Security Act
| Service | Copay |
| Doctor visits (except wellness exams, immunizations, family planning or urgent care provided at an urgent care clinic) | $3.65 per visit |
| Outpatient hospital services | $3.65 per visit |
| Speech, physical and occupational therapy | $3.65 per visit |
| Chiropractic services | $3.65 per visit |
| Podiatry services | $3.65 per visit |
| Emergency room visits for non-emergencies | $3.65 per visit |
| Federally-approved prescriptions | No copay |
Illinois
In addition to federal exclusions, the following individuals are exempt from copayments:
- Pregnant women up to 60 days after end of pregnancy
- Children younger than 19 years of age
- Individuals involved in a DCFS case
- Individuals who live in a hospital, nursing facility or intermediate care facility for people intellectual disabilities
- Individuals who live a supportive living facility or a sheltered care facility
| Service | Copay |
| Doctor visits (including chiropractors, podiatrists, optometrists, and Behavioral Health clinical services) | $3.90 |
| Prescriptions (except for insulin, AIDS drugs, chemotherapy drugs, hemophilia drugs and certain cardiovascular drugs) | $2 for generic, $3.90 for brand-name |
| Inpatient hospital services | $3.90 per day |
| Emergency room visits for non-emergencies | $3.90 |
Indiana
| Service | Traditional Medicaid Copay | Hoosier Care Connect Copay |
| Non-emergency transportation | $.50 – $2 | $1 each way |
| Emergency transportation | No copay | No copay |
| Prescriptions | $3 per prescription (generic and brand-name) | $3 per prescription (generic and brand-name) |
| Emergency room visit for non-emergencies | No copay | $3 per visit |
Iowa
In addition to federal exclusions, children younger than 21 years of age are exempt from copayments.
Copayments range from $1 to $8 depending on the managed care organization (MCO). Copayments are only charged for non-emergency use of an emergency department.
Some enrollees may be required to pay $3 monthly premiums for dental services. However, these premiums can typically be waived by completing Healthy Behaviors, an oral health assessment and preventive service tool designed to help enrollees maintain optimum oral hygiene. All dental care enrollees are required to complete Healthy Behaviors each year to continue receiving benefits. Learn more about Healthy Behaviors here: https://hhs.iowa.gov/programs/welcome-iowa-medicaid/iowa-medicaid-programs/iowa-health-and-wellness-plan/healthy-behaviors-program
Kansas
Kansas residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
Kentucky
In addition to federal exclusions, the following individuals are exempt from copayments:
- Foster children
- Pregnant women through 60 days after end of pregnancy
- Beneficiaries who have reached the 5% cost share limit for the quarter
| Service | Copay |
| Non-preventative doctor visit | $3 |
| Chiropractor | $3 |
| Podiatrist | $3 |
| Optometry | $3 |
| Visit to a rural health clinic, primary care center, or federally qualified health center | $3 |
| Inpatient hospital visit | $50 per admission |
| Dental | $3 |
| Ambulatory surgical care | $4 |
| Non-emergency visits to an emergency department | $8 |
| Physical, speech and occupational therapy | $3 |
| Durable medical equipment | $4 |
| Laboratory, diagnostic and X-ray services | $3 |
| Prescription drugs | Generic drugs $1, preferred brand name drugs $1, non-preferred brand name drugs $4 |
Louisiana
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Long-Term Care recipients
| Service | Copay |
| Prescriptions | $.50 – $3 |
Maine
In addition to federal exclusions, individuals younger than 21 years of age are exempt from copayments.
| Service | Copay |
| Outpatient hospital services | $3 |
| Inpatient hospital services | $3 per day |
| Non-emergency use of the emergency room | $3 |
| Home health services | $3 |
| Durable medical equipment | $3 |
| Private-duty nursing and personal care services | $5 per month |
| Ambulance services | $3 |
| Physical, speech and occupational therapy | $2 |
| Chiropractic and podiatry services | $2 |
| Laboratory and X-ray services | $1 |
| Optical services / Optometric services | $2 |
| Mental health clinic, substance use services and psychiatric services | $2 / $3 |
| Federally qualified and rural health services | $3 per day |
| Prescription drugs | $30 / month maximum |
Maryland
Some Medicaid enrollees may be required to make copayments for prescription medication and pharmacy services up to $3. In addition to federal exclusions, children younger than 21 years of age are exempt from copayments.
Massachusetts
Massachusetts residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
Michigan
Some Michigan residents enrolled in Medicaid are required to pay premiums, also called MIHA fees. Fees depend on family size and income. The table below includes premium amounts ranges.
| Family Size | Premium Amounts per Person |
| 1 | $21 – $29 per month |
| 2 | $14 – $19 per month |
| 3 | $12 – $16 per month |
If you have questions about your premiums or would like more information about scenarios not listed, call 1 (800) 642-3195.
Some Medicaid enrollees need to make copayments for services. In addition to federal exclusions, children younger than 21 years of age are exempt from copayments:
| Service | Copay (Income at or below 100 percent FPL) |
| Doctor visits | $2 |
| Outpatient hospital visit | $2 |
| Non-emergency visit to an emergency department | $3 |
| Inpatient hospital visit | $50 per admission |
| Prescriptions | $1 per preferred drug, $3 per non-preferred drug |
| Dental | $3 |
| Vision | $2 |
| Chiropractic services | $1 |
| Podiatry services | $2 |
| Hearing aids | $3 per aid |
Minnesota
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Members expected to be admitted for at least 30 days in a hospital, nursing facility, or intensive care unit
| Service | Copay |
| Doctor visit (excluding preventive and mental health services) | $25 per visit |
| ER visits without an admission | $75 |
| Radiology | $45 |
| Prescriptions | $7.00 generic$25.00 brand name$70.00 maximum per monthNo copays for certain mental health drugs |
| Eyeglasses | $10 |
| Inpatient Hospital | $250.00 per admission |
Mississippi
No copays apply.
Missouri
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children under 19 years of age
- Managed Care enrollees
- Members receiving Medicaid due to blindness
- Foster care participants
There is no copay required for the following services:
- Certain therapy services (physical, chemo, radiation, chronic renal dialysis) not provided as inpatient hospital service
- Medically necessary services identified through screening
- Mental health services
Some Missouri residents enrolled in Medicaid may be required to make copayments for certain services.
| Service | Copay |
| Doctor visit | $1 |
| Outpatient or emergency room services | $3 |
| Inpatient hospital care | $10 |
| Clinic services | $.50 |
| X-ray and laboratory services | $1 |
| CRNA services, Anesthesiologist assistant services | $.50 |
| Nurse practitioner services | $1 |
| Federally qualified health center or Rural health clinic services | $2 |
| Psychology services | $2 |
| Case management | $1 |
| Non-emergency medical transportation | $2 |
| Dental, optical and podiatry services | $.50 – $3 |
Montana
Montana residents enrolled in the HELP Medicaid Plan (also known as Medicaid Expansion) are required to pay monthly premiums.
Montana residents enrolled in Medicaid or the HELP Medicaid Plan do not pay any copayments for services.
Nebraska
In addition to federal exclusions, the following individuals are exempt from copayments:
- Members in alternative care facilities
- Members who are State Disability Program recipients
- Members who are Home and Community-Based Medicaid Waiver recipients
| Service | Copay |
| Prescriptions (except birth control) | $2 per generic, $3 per brand-name |
| Physician visit (except family practice or general practice, pediatricians, internists, nurse practitioners, nurse midwives and physician assistants) | $2 per visit |
| Outpatient hospital | $3 per visit |
| Inpatient hospital | $15 per admission |
| Mental health and substance abuse treatment | $2 per service |
| Physical and occupational therapy | $1 per visit |
| Speech therapy | $2 per visit |
| Chiropractic and podiatry services | $1 per visit |
| Vision | $2 per visit/exam |
| Dental | $3 per service |
| Durable medical equipment | $3 per service |
| Eyeglasses | $2 per pair |
| Hearing aids | $3 per aid |
Nevada
Nevada residents enrolled in Medicaid do not pay any copayments for services.
New Hampshire
In addition to federal exclusions, members with incomes below 100 percent of the federal poverty level (FPL) are exempt from copayments:
Enrollees with incomes over 100 percent of the FPL have to make copayments for prescriptions. There is a $147 copayment maximum per quarter. Once an enrollee pays $147 in a three-month span, he or she is exempt from copayments for the remainder of the quarter. The quarter schedule is as follows:
- Quarter 1: January 1 – March 31
- Quarter 2: April 1 -June 30
- Quarter 3: July 1 – September 30
- Quarter 4: October 1 – December 31
| Service | Copay |
| Generic prescriptions | $1 |
| Brand-name prescriptions | $2 |
New Jersey
Adult New Jersey residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
Copayments are required for children age 18 and under if their household income is above 150 percent of the federal poverty level (FPL). If a child qualifies, they must also pay monthly premiums according to the following scale:
- 0 to 200 percent of the FPL: $0
- 200 to 250 percent of the FPL: $42.50
- 250 to 300 percent of the FPL: $85.00
- 300 to 350 percent of the FPL: $142.50
These amounts are the same by household regardless of how many children in the household participate in the program.
New Mexico
New Mexico residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
New York
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Pregnant women up to two months after end of pregnancy
- Members living in a nursing home
- Members with incomes below 100 percent of the federal poverty level (FPL)
- Members residing in an adult care facility licensed by the New York State Department of Health
- Members in an Office of Mental Health (OMH) or Office for People with Developmental Disabilities (OPWDD) certified community residence
- Members involved in Comprehensive Medical Case Management (CMCM) or Services Coordination Program
- Members involved in the Home and Community Based Services (HCBS) or Traumatic Brain Injury (TBI) waiver programs
| Service | Copay |
| Prescriptions | $1 per generic or brand name preferred / $3 per brand-name non-preferred |
| Over-the-counter drugs | $.50 per drug |
| Clinic visits | $3 per visit |
| Inpatient hospital visit | $25 |
| Laboratory services from independent clinical lab or hospital-based / free standing clinic lab | $.50 per test |
| Non-emergency use of an emergency department | $3 per visit |
| Medical supplies | $1 per claim |
| Private practicing physician services (including laboratory and/or x-ray services, home health services, personal care services or long-term home health care services), Psychotropic and tuberculosis drugs | No copay |
North Carolina
In addition to federal exclusions, Children younger than 21 years of age are exempt from copayments.
| Service | Copay |
| Prescriptions | $4 per generic and brand-name |
| Doctor visit | $4 per visit |
| Dental | $3; only one copay required for services requiring more than one visit |
| Optometry | $4 per visit |
| Optical supplies and services | $2 per pair |
| Outpatient visits | $3 per visit |
| Psychiatric and psychological care | $3 per visit |
| Chiropractic care | $4 per visit |
| Podiatry | $4 per visit |
| Non-emergency use of an emergency department | $4 per visit |
North Dakota
North Dakota residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
Ohio
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Pregnant women up to 90 days after end of pregnancy (must still pay copayments for routine eye exams and eyeglass fittings)
- Members in a managed care plan that does not charge copayments
- Members living in nursing homes
| Service | Copay |
| Prescriptions | $2 per brand-name drugs, $3 per drug requiring prior authorization |
| Non-emergency use of an emergency department | $3 per visit |
| Eye exams | $2 per exam |
| Eyeglasses | $1 per fitting |
| Dental services | $3 per visit |
Oklahoma
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Members living in nursing homes
Any members who have copays will not have to pay more than 5 percent of their monthly household income on copayments. Once they reach this amount, they will not have to pay any more copayments for the month.
| Service | Copay |
| Prescriptions | $4 per prescription |
| Doctor visits, including specialists and podiatry | $4 per visit |
| Outpatient services | $4 per visit |
| Inpatient services | $10 per day for the first seven days, $5 per day after for a maximum of $75 |
| Home health care | $4 per visit |
| Laboratory and X-ray services | $4 per visit |
| Physical, occupational and speech therapy | $4 per visit |
| Behavioral health and substance abuse treatment services | $3 per visit; $10 per day up to a $75 maximum for inpatient behavioral treatment |
| Chemotherapy and radiation therapy | $4 per visit |
| Clinic services including dialysis | $4 per visit |
| FQHC and rural health clinic services | $4 per visit |
| Home health services | $4 per visit |
| Diabetic supplies | $4 per claim |
| Immunizations | $4 per date of service |
| Durable medical equipment | $4 copay when prescribed by a medical provider and requiring prior authorization |
| Tuberculosis services | $4 per visit |
Oregon
Oregon’s Medicaid program does not require copays.
Pennsylvania
In addition to federal exclusions, the following individuals are exempt from copayments:
- Residents of long term care facilities
- Individuals in the Title IV-B Foster Care and IV-E Foster Care and Adoption Assistance Programs
| Service | Copay |
| Prescriptions | $1 per generic, $3 per brand-name |
| Inpatient hospital visit | $3 per day; $21 maximum per visit |
| Non-preventative physician visit | $0.65 or $3.80 depending on if below or above FPL |
| X-ray or radiation treatment | $1 per test |
| Outpatient psychotherapy services | $.50 per service |
| Laboratory services, Home health agency services, Psychiatric partial hospitalization program services, Renal dialysis services, Blood and blood products, Oxygen, Ostomy supplies, Durable medical equipment rental | No copay |
For other services requiring copayment, the amount will be the following:
| Cost to Medicaid Program | Copayment Amount |
| $2 – $10 | $.65 |
| $10.01 – $25 | $1.30 |
| $25.01- $50 | $2.55 |
| $50.01 or more | $3.80 |
Rhode Island
Rhode Island residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
South Carolina
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 19 years of age
- Individuals in a nursing facility or ICF-MR
- Members of the Health Opportunity Account (HOA) program
Copayments are not required for the following services:
- Medical equipment and supplies provided by DHEC
- Orthodontic services provided by the DHEC
- End stage renal disease (ESRD) services
- Infusion center services
- Waiver services
| Service | Copay |
| Doctor visits | $3.30 per visit |
| Anesthesiologist | $3.30 |
| Clinic visits | $3.30 per visit |
| Non-emergency outpatient hospital care | $3.40 per visit |
| Inpatient hospital care | $25 per admission |
| Outpatient hospital (non-emergency) | $3.40 per claim |
| Prescriptions | $3.40 each |
| Home health services | $3.30 per visit |
| Dental care | $3.40 per visit |
| Optometrist services | $3.30 per visit |
| Chiropractic and podiatry care | $1.15 per visit |
| Durable medical equipment and supplies | $3.40 per claim |
| FQHC and rural health clinic | $3.30 per visit |
South Dakota
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Members living in a long-term care facility or receiving home and community-based services
| Service | Copay |
| Doctor visits | $3 per visit |
| Chiropractic services | $1 per procedure |
| Prescriptions | $1 per generic, $3.30 per brand-name |
| Outpatient hospital care | 5 percent of allowable amount; maximum $50 |
| Inpatient hospital care | $50 per admission |
| Independent mental health practitioners | $3 per procedure |
| Mental health clinics | 5% of allowable reimbursement |
| Dental care (including dentures) | $3 per procedure / $3 per denture |
| Optometric Services and Optical Supply | $2 per visit or procedure |
| Ambulatory surgical care | 5 percent of allowable amount; maximum $50 |
| Diabetes education | $3 per unit of service / visit |
| Nutrition services | $2 per day for enteral and $5 per day for parenteral |
| Optometric services and supply | $2 per visit and $2 per procedure |
| Podiatry care | $2 per visit |
| Chiropractic care | $1 per procedure |
| Mental health clinic | 5 percent of allowable amount |
| Independent mental health practitioner | $3 per visit |
| Durable medical equipment, supplies and prosthetic devices | 5 percent of allowable reimbursement amount |
Tennessee
Individuals enrolled in Tennessee Medicaid who are below the federal poverty level (FPL) only have copayments for some prescriptions. The following prescriptions do not have copayments:
- Prescriptions from hospice care
- Birth control
- Children on Medicaid whose family income is below 100% of the federal poverty level
line - Medication prescribed during emergency care
- Medicine prescribed for pregnant women
| Service | Copay | ||
| 0-133% FPL | 134-199% FPL | 200% + FPL | |
| Generic prescriptions | $1.50 each | ||
| Brand-name prescriptions | $3 each | ||
| Hospital ER (waived if admitted) | $0 per visit | $8.20 per visit | $50 per visit |
| Primary care provider and community mental health agency services other than preventative care | $0 per visit | $5 per visit | $15 per visit |
| Physician specialists including psychiatrists | $0 per visit | $5 per visit | $20 per visit |
| Inpatient hospital admission (waived if readmitted within 48 hours for the same episode) | $0 per visit | $5 per visit | $100 per visi |
Texas
Texas residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
Utah
In addition to federal exclusions, members in the Medicaid Cancer Program are exempt from copayments.
| Service | Copay |
| Doctor visits, podiatry and outpatient hospital services | $4 per visit; maximum $100 per year |
| Prescriptions | $4 per prescription; maximum $20 per month |
| Non-emergency use of an emergency department | $8 per visit |
| Inpatient hospital visit | $75 per admission |
| Vision care | $4 per optometrist visit |
Vermont
In addition to federal exclusions, individuals living in nursing homes are exempt from copayments.
| Service | Copay |
| Prescriptions | $1 – $3 |
| Dental care | $3 per visit |
| Outpatient hospital care | $3 per day |
| Sexual assault-related services | No copayment |
Virginia
In addition to federal exclusions, children younger than 21 years of age are exempt from copayments.
| Service | Copay |
| Prescriptions | $1 per generic, $3 per brand-name |
| Physician office visit | $1 per visit |
| Other physician visit | $3 per visit |
| Outpatient hospital visit | $3 per visit |
| Inpatient hospital visit | $100 per admission |
| Clinic visit | $1 per visit |
| Home health care | $3 per visit |
| Eye exam | $1 per examination |
| Rehabilitation services | $3 per visit |
Washington
Washington residents enrolled in Medicaid do not pay any copayments or out-of-pocket costs for services.
West Virginia
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Members living in nursing homes
| Service | Copay | ||
| Up to 50% FPL with max of $8 out of pocket | 50.01 – 100% FPL with max of $71 out of pocket | 100.01% FPL + with max of $143 out of pocket | |
| Prescriptions | $0 – $3 | ||
| Doctor visit | $0 per visit | $2 per visit | $4 per visit |
| Inpatient visit | $0 per visit | $35 per visit | $75 per visit |
| Non-emergency use of an emergency department | $8 per visit | ||
| Outpatient surgical services | $0 per visit | $2 per visit | $4 per visit |
| Intermediate Care Facility or MR Services | No copayment | ||
Wisconsin
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 19 years of age
- Children in foster care or adoption assistance
- Pregnant women up to 60 days after end of pregnancy
- Members living in nursing homes
- Members who enroll by Express Enrollment
| Amount of Service | Copay |
| Up to $10 | $.50 |
| $10.01 – $25 | $1 |
| $25.01 – $50 | $2 |
| More than $50 | $3 |
Wyoming
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 19 years of age
- Members living in nursing homes
| Service | Copay |
| Generic prescriptions | $.65 each |
| Brand-name prescriptions | $3.65 each |
| Office & home visits | $2.45 per visit |
| Eye exams | $2.45 |
| Rural health center visits | $3.65 |
| Federally qualified health center visits | $3.65 |
U.S. Territories
American Samoa
American Samoa residents enrolled in Medicaid do not pay any copayments for services, but hospitals may charge separate fees for service.
Guam
Guam residents enrolled in Medicaid do not pay any copayments for services.
Commonwealth of Northern Mariana Islands (CNMI)
CNMI residents enrolled in Medicaid do not pay any copayments for services.
Puerto Rico
In addition to federal exclusions, the following individuals are exempt from copayments:
- Children younger than 21 years of age
- Pregnant women up to 60 days after end of pregnancy
- Individuals with incomes at or below 50 percent FPL
- Members living in nursing homes
| Service | Copay |
| Generic prescriptions | $1 each |
| Brand name prescriptions | $3 each |
| Doctor visit (primary care or specialist) | $1 per visit |
| Physical, occupational and respiratory therapy | $1 per procedure |
| Inpatient visit | $4 – $8 per admission |
| Dental care | $1 per visit |
| Laboratory and X-ray services | $.50 per procedure |
| Non-emergency use of an emergency department | $4 – $8 per visit |
U.S. Virgin Islands
Information for Medicaid cost sharing for the U.S. Virgin Islands is not readily available. For more information, contact the Medicaid office at (340) 715-6929.
Dual Eligibility in Medicare and Medicaid

Some individuals can receive benefits from both Medicaid and Medicare. They are called dual eligible recipients. Dual eligibility affects how medical expenses are billed.
Who qualifies for dual eligibility?
Generally, individuals can be dual eligible if they are over 65 years of age and meet the work requirements for Medicare, while also meeting the income and/or disability requirements for Medicaid.
Individuals with disabilities or late-stage renal failure and low household incomes may also qualify for both Medicare and Medicaid.
How Dual Eligibility Affects Billing
Individuals who qualify for both Medicare and Medicaid will have most benefits covered first by Medicare, then by Medicaid. For instance, if someone receives coverage through Medicare but incurs personal costs or exceeds the Medicare requirements, Medicaid benefits will cover some or all of the expenses.
Some individuals are classified as partial dual, while others are classified as full dual.
Partial-dual eligible individuals are generally eligible for full Medicare benefits, but their incomes will only allow them to receive partial Medicaid benefits with additional costs and copayments. Full-dual eligible individuals will qualify for full benefits from both programs, reducing the amount of cost-sharing they will have to cover.
Your Medicaid Card
When you receive Medicaid benefits, you will be issued a Medicaid card that allows you to obtain access to benefits and Medicaid coverage.
What is a Medicaid card?
A Medicaid card is a card documenting that you are currently eligible for Medicaid benefits. All Medicaid beneficiaries receive a card. Depending on the state, your card may contain any of the following information:
- Your name
- Your state of residence
- Your state’s health department
- Your Medicaid ID Number
- Your Medicaid card number
- Your Medicaid card date of issuance
- Your health insurance policy or plan
- Your primary care doctor’s name
- Your pharmacy of choice
You can only share your Medicaid card number with a Medicaid provider who is providing services to you. Sharing it with anyone else is considered Medicaid fraud. Your benefits will be revoked, and you may be charged a fine or issued a prison sentence of up to 10 years if found guilty of committing Medicaid fraud.
How to Use the Medicaid Card
When you visit a doctor or seek medical services, you can present the Medicaid card in order to receive coverage for your treatment.
It’s a good idea to check if an organization accepts Medicaid before seeking treatment. You can find out where to obtain treatment by contacting the member services phone number on the back of your card.
Replacing a Medicaid Card
If you lose your Medicaid card or it is severely damaged, you should replace it as soon as possible. It can be difficult to obtain benefits without the card and card number.
When to Replace
You should replace a Medicaid card when it is:
- Lost
- Stolen
- Severely damaged and illegible
How to Replace
To replace a lost, stolen or damaged Medicaid card, you should contact your state’s Medicaid agency and request a replacement. Provide any required information, including your name, Social Security Number and residential address to confirm your identity and request the card.
Visit the section titled “Medicaid Contact Information By State and Territory” to find contact information for your state’s Medicaid agency.
Annual Limits
Prior to the passage of the Affordable Care Act (ACA), insurance plans could impose an annual limit on the benefits they would pay out for an individual. Following the ACA’s passage, annual limits on essential health benefits were banned.
Although some plans have been grandfathered into the new law and can continue to impose annual limits, all plans issued from January 1, 2014 onward have no limits.
- Plans that begin between September 23, 2010 and September 22, 2011 cannot limit essential benefit coverage to anything less than $750,000 annually.
- Plans that begin between September 23, 2011 and September 22, 2012, essential benefits cannot be limited to less than $1.25 million annually.
- Plans that begin between September 23, 2012 and January 1, 2014 cannot restrict essential benefits to less than $2 million annually.
- All plans that begin after January 1, 2014 can have no annual limits on essential benefits.
Plans can limit non-essential benefits.
Alternative Sources of Subsidized Health Insurance

If you cannot obtain health insurance coverage through Medicaid, you can find other sources of subsidized health insurance to ease the burden of health care costs.
Basic Health Programs
States have the option to implement Basic Health Programs (BHPs) to complement Medicaid programs for individuals who would otherwise not be able to afford a plan through the Marketplace. If you do not currently qualify for Medicaid, you may be eligible for coverage through a BHP.
BHPs provide coverage for citizens and qualified residents whose incomes are between 133 percent and 200 percent of the federal poverty level. They also provide coverage for individuals whose incomes fall below 133 percent of the FPL and cannot obtain Medicaid due to their citizenship status.
All BHPs provide the ten essential benefits as outlined by the Medicaid program and the ACA. As of 2020, Minnesota and New York have implemented BHPs.
Children’s Health Insurance Program (CHIP)
The Children’s Health Insurance Program (CHIP) provides comprehensive free or low-cost healthcare benefits to children whose parents or guardians do not qualify for Medicaid. CHIP is a federal program, and each state/territory has the flexibility to design its own CHIP program within federal guidelines. Therefore, CHIP benefits may differ in each state/territory.
CHIP benefits may include annual check-ups, hospital visits, dental insurance, vision insurance and more. All services are provided through medical providers that participate in the CHIP program. Not all doctors and medical facilities accept CHIP patients.
Learn more about the Children’s Health Insurance Program with our free guide here.









